REVIEW ARTICLE
KNOWLEDGE, ATTITUDES AND PRACTICES OF
UNIVERSITY STUDENTS ON HPV AND CERVICAL CANCER PREVENTION: INTEGRATIVE REVIEW
CONHECIMENTOS, ATITUDES E PRÁTICA DE
UNIVERSITÁRIAS SOBRE PREVENÇÃO DO HPV E CÂNCER CERVICAL: REVISÃO INTEGRATIVA
CONOCIMIENTOS, ACTITUDES Y PRÁCTICAS DE
ESTUDIANTES UNIVERSITARIAS SOBRE LA PREVENCIÓN DEL VPH Y EL CÁNCER DE CUELLO
UTERINO: REVISIÓN INTEGRADORA
https://doi.org/10.31011/reaid-2026-v.100-n.1-art.2598
1Rawane
Soares Santos
2José
Cláudio Garcia Lira Neto
3Jardeliny
Corrêa da Penha
4José
Ribamar Lopes Batista Júnior
5Maria
Augusta Rocha Bezerra
1Universidade
Federal do Piauí (UFPI), Floriano, Brazil. Orcid: https://orcid.org/0000-0003-1253-7510
2Universidade
Federal do Piauí (UFPI), Floriano, Brazil. Orcid: https://orcid.org/0000-0003-2777-1406
3Universidade
Federal do Piauí (UFPI), Floriano, Brazil. Orcid: https://orcid.org/0000-0001-5956-9072
4Universidade
Federal do Piauí (UFPI), Floriano, Brazil. Orcid: https://orcid.org/0000-0002-4777-3305
5Universidade
Federal do Piauí (UFPI), Floriano, Brazil. Orcid: https://orcid.org/0000-0003-0472-1852
Autor
correspondente
Rawane
Soares Santos
Universidade
Federal do Piauí, Campus Amílcar Ferreira Sobral, BR 343, Km 3,5, Bairro
Meladão, Floriano- PI. Brazil. CEP: 64.808-605. Phone: +55(89)99423-0177 –
E-mail: rawanessantos@gmail.com
Submission: 11-06-2025
Approval: 04-12-2025
ABSTRACT
Introduction: Cervical cancer (CC) is a global
public health problem due to its high incidence and mortality rates. In
addition, the lack of accurate and comprehensive information on the subject can
lead people to engage in risky behaviors. Objective: To identify knowledge,
attitudes and practices of university students regarding the prevention and
control of Human Papillomavirus (HPV) and cervical cancer. Methods: This is an
integrative review, carried out in October 2024, with searches in the following
databases: MEDLINE via Pubmed, Latin American and Caribbean Literature in
Health Sciences and Base de Dados em Enfermagem, using
controlled and uncontrolled descriptors selected from the Health Sciences
Descriptors and Medical Subject Headings. Results: The final sample consisted
of 19 studies. It was found that the students have adequate knowledge about HPV
and CC, risk factors, means of transmission and prevention and screening
methods, however, gaps remain regarding clinical manifestation, HPV infection,
diagnostic methods and vaccination. Regarding attitudes and practice, the
students have favorable attitudes towards early detection through
cytopathological examination, however, they presented unsatisfactory practices
in relation to cytopathological examination and vaccination. Conclusion: There
is a need for more comprehensive and investigative educational strategies to be
implemented, especially in the university context, to promote proactive
attitudes and health practices that minimize vulnerability to the Human
Papillomavirus and cervical cancer.
Keywords: Health Knowledge,
Attitudes, Practice; Human Papillomavirus Viroses; Uterine Cervical Neoplasms; Students.
RESUMO
Introdução: O câncer de colo uterino (CCU) é um problema de saúde
pública mundial devido às suas altas taxas de incidência e mortalidade. Além
disso, a ausência de informações precisas e abrangentes sobre o tema pode levar
as pessoas a se exporem a comportamentos de risco. Objetivo: Identificar
conhecimentos, atitudes e prática de estudantes universitárias sobre a
prevenção e controle do Papilomavírus Humano (HPV) e do câncer de colo uterino.
Métodos: Trata-se de revisão integrativa, realizada em outubro de 2024, com
busca nas bases de dados: MEDLINE via Pubmed, Literatura Latino-Americana e do
Caribe em Ciências da Saúde e Base de Dados em Enfermagem, utilizando
descritores controlados e não controlados selecionados dos Descritores de
Ciências da Saúde e Medical Subject Headings. Resultados: A amostra final foi
composta por 19 estudos. Verificou-se que as estudantes têm conhecimento
adequado sobre HPV e CCU, fatores de risco, meios de transmissão e métodos de
prevenção e rastreamento, entretanto, ainda persistem lacunas relativas à
manifestação clínica, à infecção por HPV, aos métodos de diagnóstico e à
vacinação. No que tange às atitudes e prática, as estudantes possuem atitudes
favoráveis quanto à detecção precoce por meio do exame citopatológico, contudo,
apresentaram práticas insatisfatórias em relação ao exame citopatológico e à
vacinação. Conclusão: Observa-se a necessidade de que estratégias educativas
mais abrangentes e investigativas sejam implementadas, especialmente no
contexto universitário, para promover atitudes proativas e práticas de saúde
que minimizem a vulnerabilidade frente ao Papilomavírus Humano e câncer de colo
uterino.
Palavras-chave: Conhecimentos, Atitudes e Prática em Saúde; Papillomavirus Humano;
Neoplasias do Colo do Útero; Estudantes.
RESUMEN
Introducción: El cáncer cervicouterino (CCU) es
un problema de salud pública mundial debido a su alta incidencia y mortalidad.
Además, la falta de información precisa y completa sobre el tema puede llevar a
las personas a exponerse a conductas de riesgo. Objetivo: Identificar los
conocimientos, actitudes y prácticas de estudiantes universitarios respecto a
la prevención y el control del Virus del Papiloma Humano (VPH) y el cáncer
cervicouterino. Métodos: Se realizó una revisión integrativa en octubre de 2024,
con búsquedas en las siguientes bases de datos: MEDLINE vía Pubmed, Literatura
Latinoamericana y del Caribe en Ciencias de la Salud y la Base de Datos de
Enfermería, utilizando descriptores controlados y no controlados seleccionados
de los Descriptores de Ciencias de la Salud y Medical Subject Headings.
Resultados: La muestra final consistió en 19 estudios. Se encontró que los
estudiantes poseen conocimientos adecuados sobre el VPH y el CaCu, sus factores
de riesgo, vías de transmisión y métodos de prevención y cribado; sin embargo,
aún existen lagunas en cuanto a las manifestaciones clínicas, la infección por
VPH, los métodos de diagnóstico y la vacunación. En cuanto a las actitudes y
prácticas, los estudiantes muestran una actitud favorable hacia la detección
temprana mediante el examen citopatológico; sin embargo, presentaron prácticas
insatisfactorias con respecto al examen citopatológico y la vacunación.
Conclusión: Es necesario implementar estrategias educativas más integrales e
investigativas, especialmente en el contexto universitario, para promover
actitudes proactivas y prácticas de salud que minimicen la vulnerabilidad al
Virus del Papiloma Humano y al cáncer de cuello uterino.
Palabras clave: Conocimientos,
Actitudes y Práctica en Salud; Virus del Papiloma Humano; Neoplasias del Cuello
Uterino; Estudiantes.
INTRODUCTION
Human Papillomavirus
(HPV) is a DNA virus from the Papillomaviridae family, consisting of more than
170 types divided into low-risk and high-risk HPV. Low-risk viruses are
associated with common clinical manifestations, such as genital warts. In turn,
those considered high-risk (16, 18, 31, 45, among others) are related to
precancerous lesions and the development of cervical cancer (CCU),(1,2)
with HPV16 and HPV18 subtypes being responsible for more than 70.0% of cases of
this neoplasm.(2)
The incidence of CCU was
approximately 660,000 cases worldwide, with more than half having negative
outcomes, such as deaths. Because of this, cervical cancer has become the
fourth most frequent and lethal cancer in the world among women.(3)
In Brazil, in 2023, the incidence exceeded 17,000 cases and six thousand deaths
were recorded.(4)
The women most affected
by cervical cancer were those residing in developing regions, such as Brazil,
and more specifically, in areas with less access to healthcare, such as the
North and Northeast regions of the country. Exposure to risk factors, barriers
to effective prevention, early diagnosis, and curative treatment are directly
related to mortality from this type of cancer.(3)
Therefore, it is
important that women, especially those exposed to sexually transmitted
infections, possess adequate knowledge, attitudes, and practices regarding the
prevention and control of HPV and cervical cancer, which is possible through
the development of comprehensive healthcare and health education actions.
In the meantime, the
literature revealed studies conducted internationally, in Brazil, and
specifically in the Northeast, that address the prevention and control of HPV
and CCU among female university students.(5-7) Thus, this research
seeks to answer the following research question: what are the knowledge,
attitudes, and practices of female university students regarding the prevention
and control of HPV and CCU?
Therefore, the objective
was to identify the scientific evidence regarding the knowledge, attitudes, and
practices of female university students about the prevention of HPV and CCU.
METHODS
This is an integrative
review, conducted in six stages: 1) development of the guiding question; 2)
search and selection of primary studies; 3) data extraction from the studies;
4) critical appraisal of the primary studies included in the review; 5) synthesis
of the review results; and 6) presentation of the method.(8)
For the formulation of
the guiding question, the PICo strategy was used (P: university students; I:
knowledge, attitudes and practice; Co: HPV and CCU prevention). Thus, the
following question was defined: What are the knowledge, attitudes and practices
of university students regarding HPV and CCU prevention?
The bibliographic survey,
that is, the search for primary studies, was carried out in the following
databases: MEDLINE via PUBMED, Latin American and Caribbean Literature in
Health Sciences (LILACS), and Nursing Database (BDENF), using controlled
descriptors from the Health Sciences Descriptors (DeCS) and Medical Subject
Headings (MeSH). To identify the largest number of publications, controlled and
uncontrolled descriptors and the Boolean operators AND and OR were used to
establish the study search strategy (Table 1).
Table 1 - Search strategy for primary
studies in the selected databases.
|
Database
|
Search Strategy
|
Results
|
|
PUBMED
|
("University Students" OR "College Students"
OR "Undergraduate Students" OR "Students") AND
("Health Knowledge, Attitudes, Practice" OR "CAP Surveys"
OR "CAP" OR "KAP") AND ("HPV" AND "Uterine
Cervical Neoplasms" OR "Cervical Cancer" OR "Uterine
Cervical Cancer" OR "Cervical neoplasm")
|
301
|
|
LILACS
|
13
|
|
BDENF
|
4
|
Source: Prepared by the authors
(2024).
For the selection of
primary studies, the following inclusion criteria were adopted: scientific
articles, of the observational type, available in full, free of charge, in
English, Portuguese, or Spanish, published between 2014 and 2024, and that
answered the guiding research question. Studies that addressed knowledge,
attitudes, or practice separately were also included. Duplicate articles,
qualitative articles, and review articles were excluded.
Regarding the selection
of primary studies, it should be noted that the titles and abstracts were read,
followed by the application of eligibility criteria. After this, the final
sample of articles that were read in full was defined.
For data collection, the
stage involving the extraction of data from the studies, a spreadsheet was used
in Google Sheets, containing the following information: article title, authors,
journal, country, year of publication, approach and design of the article,
level of evidence, objective, sample, participants' courses of study, questions
about knowledge, attitudes and practice, and main results. Subsequently, a
critical appraisal of the primary studies included in the review was carried
out.
For the assessment of
the level of evidence, the JBI classification was used, which separates levels
into: level I: systematic review or meta-analysis; level II: randomized
controlled trial; level III: non-randomized controlled trial/quasi-experimental
studies; level IV: well-designed cohort or case-control studies; level V:
systematic review of qualitative and descriptive studies; level VI: descriptive
or qualitative studies; and level VII: authoritative opinion or expert report.
The levels are classified as strong (I and II), moderate (III to V) and weak
(VI to VII).(9)
The data analysis was
based on content analysis of the selected studies, in which their respective
results were classified into categories that allowed inference about the
knowledge, attitudes and practices of university students in the prevention and
control of HPV and cervical cancer.
Approval from the
Research Ethics Committee (REC) and the Free and Informed Consent Form (FICF)
were waived for this study, as it is a literature review and all data used were
in the public domain.
RESULTS
Based on the database
search, 318 records were identified. After excluding duplicates and reading
titles and abstracts, 30 articles were read in full; of these, 19 articles were
selected to compose the final sample of the review. Figure 1 presents the flowchart
for selecting the studies included in the integrative review.
Figure
1 -
Flowchart of the process for selecting studies included in the review.
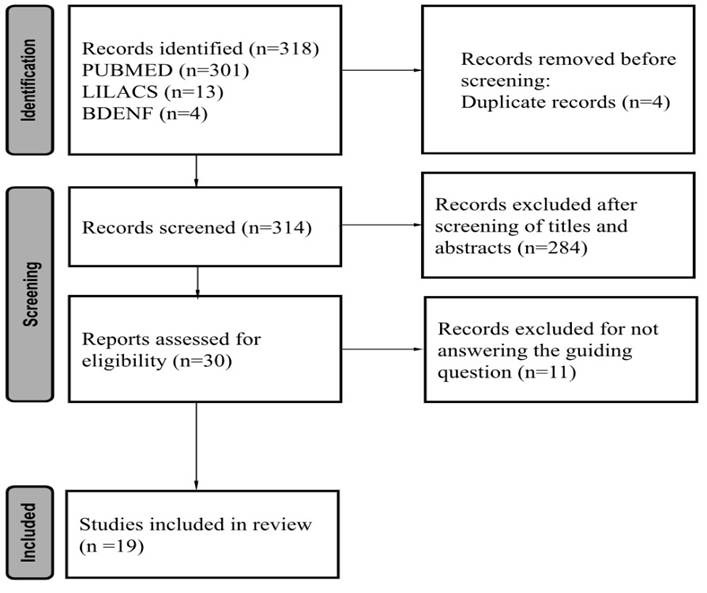
Source: Prepared by the
authors (2024).
Among the studies
included in the review, the majority, 18 (94.7%), were published in English
between 2014 and 2024, with the highest frequency of publication in 2016
(26.3%), followed by 2014 (15.8%). Regarding the place of publication, Turkey
contributed three (15.8%) publications, followed by India, China, Brazil, Saudi
Arabia, and Ethiopia, all of which had two (10.5%) publications (Figure 2).
Figure 2 - Characteristics of the
evidence included in the study.
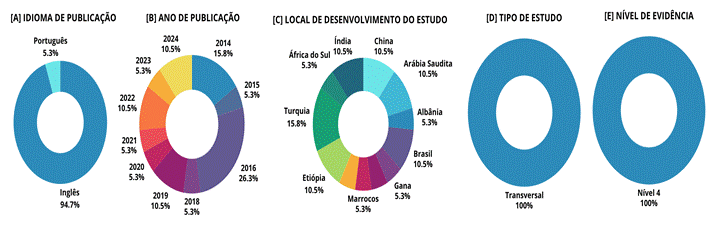
[A] Language of
publication; [B] Year of publication; [C] Location where the study was
conducted; [D] Type of study; and [E] Assessment of the level of evidence of
the studies included in the review.
Source: Prepared by the
authors (2025).
Table 2 presents the
characterization of the research sample, which ranged from 76 to 2,679
participants, with the population consisting of female and male university
students, as well as the main results related to the knowledge, attitudes,
and/or practices of university students regarding the prevention of cervical
cancer and HPV. Regarding the study types, all were characterized as
cross-sectional studies (100%), indicating a low level of scientific evidence
(LE IV).
Table 3 presents a
compilation of questions about knowledge, attitudes, and practices present in
the studies.
Table 3 - Questions about knowledge,
attitudes, and practices from the studies included in the review.
|
Knowledge
|
Attitudes
|
Practice
|
|
Have you ever heard of cervical cancer? 7 9 14 15 17-19 21
23
|
Where did you get your information about cervical cancer? 9
15 23
|
Should only teenage girls receive the HPV vaccine? 7
|
Have you already received the HPV vaccine? 7 9 15 18 19
|
|
What are the causes of cervical cancer? 7 17 21
|
What are the risk factors for cervical cancer? 9 12 15
17-19 21 22 24 25
|
Would you be embarrassed to have a Pap smear?? 9
|
|
Is there any association between HPV and cervical cancer? 7
14
|
What are the diagnostic methods for cervical cancer? 9 16
18 19
|
Do you think Pap smears are painful? 9
|
Have you ever had an HPV test? 9
|
|
What are the main types of HPV that cause cancer? 7 10 18
20
|
Have you ever heard of a Pap smear?? 9 11 12 18 20-22
|
Do you think that fear of the test result is a inhibiting
factor?? 9
|
|
Does HPV cause genital warts? 7 8 10 11 13 18 19 24
|
At what age should cervical cancer screening begin? 9 15 21
|
Do you think condoms prevent HPV infection? 9
|
Have you ever had a Pap smear?? 12 15 19 21
|
|
Have you heard about the HPV vaccine? 7-9 13 18 19 23
|
How often should a Pap smear be done?? 9 11 15 21 22
|
Do you think cervical cancer is a terminal illness? 12 15
|
|
Do you know the names of the HPV vaccines? 7 20
|
Can HPV cause HIV/AIDS? 10 18
|
Do you think cervical cancer can be sexually transmitted?
12
|
Why haven't you had a Pap smear yet?? 15
|
|
Who is eligible to receive the HPV vaccine? 7 19 20 23
|
Can HPV be cured with antibiotics? 10 16 18
|
Do you think cervical cancer is curable?? 12
|
|
Have you ever heard of HPV? 8 11 13 14 19 20
|
Do most sexually active people contract HPV at some point in
their lives? 10 16 18
|
Do you think cervical cancer can cause infertility? 18 23
|
At what age did you have sexual intercourse for the first time? 9
15
|
|
Is HPV sexually transmitted? 8 10 13 16 18 24
|
HPV usually requires treatment.? 10 18
|
Do you believe that all women are at risk of cervical cancer?
12 15
|
How many sexual partners have you had? 9 15
|
|
Does HPV cause cervical cancer? 8 10 11 13 16 18 19 24
|
Does the HPV vaccine offer protection against genital warts? 10
18
|
Do you plan to have a Pap smear in the future? 12 15
|
|
Can HPV infect both men and women? 8 13 16 19 20 24
|
Does the HPV vaccine offer protection against all sexually
transmitted infections? 10 18
|
Do you believe you have a chance of developing cervical cancer? 15
18
|
Have you had cervical cancer screening in the last 3 years?
21
|
|
HPV infection can occur without symptoms.? 8 10 13 14 18 20
|
What are the symptoms identified in cervical cancer?? 12 15
17 19 21 22 24
|
Do you think there are effective methods to reduce the risk of
cervical cancer? 15 18
|
|
HPV can cause other types of genital cancer (penis, anus)?
8 13
|
Do you think HPV infection is the main cause of cervical
cancer?? 14 18
|
Do you think cervical cancer can be treated? 15
|
Do you use condoms during sexual intercourse? 9
|
|
What health problems are associated with HPV? 8 13 14 20
|
What is the causative agent of cervical cancer?? 15
|
Do you think the vaccine offers lifelong protection against HPV?
19
|
|
What are the methods for preventing HPV? 8 9 13-1 17-19 21
|
Can cervical cancer be cured in its early stages? 15
|
Do you believe that cervical cancer can be prevented with a
vaccine?? 19 21
|
Did you use a condom the last time you had sex? 9
|
|
What are the modes of transmission for HPV? 8 13 17 19 20
21
|
How can cervical cancer be treated? 15 21
|
|
Does the HPV vaccine protect against cervical cancer? 8-10
13 18
|
Is cervical cancer a terminal illness? 18
|
|
Once vaccinated, do women need to be screened for cervical
cancer? 8 10 13 18 20
|
Where did you get your information about HPV? 19
|
Do you think there is a need for better education about HPV and
related diseases? 20
|
What is the reason why you don't use a condom when you have sex?
9
|
|
Is the HPV vaccine only for sexually active people? 8 13
|
Can cervical cancer be prevented? 22
|
Do you want to learn more about HPV and its related diseases?? 20
|
You return to the doctor's office to have your Pap smear results
collected.? 11
|
|
A vacina contra o HPV deve ser administrada antes da primeira
relação sexual? 8 10 13 18 24
|
Para quê o teste de Papanicolau é realizado? 20 25
|
Source: Prepared by the authors (2024).
DISCUSSION
The studies included in
this review demonstrate that, although many participants have a general
knowledge considered adequate regarding the prevention and control of HPV and
cervical cancer(9-12,15,18,19,20,24) significant gaps are observed
in relation to specific aspects. Many participants revealed incipient or
erroneous knowledge about symptoms, modes of HPV transmission, diagnostic
methods and, in some cases, believed that there was no vaccine against HPV or
that it was not effective in preventing cervical cancer.(8,17,19)
This limitation in knowledge is worrying, as it indicates that general
information on the subject alone is not sufficient to promote effective
behavioral changes or ensure adequate prevention.
In contrast, other
studies have found that research participants possessed adequate knowledge
about HPV and its association with cervical cancer and other pathologies, knew
the risk factors and modes of transmission, and were familiar with
cytopathological examination as a screening method and the frequency with which
it should be performed, and recognized the effectiveness of HPV vaccines in
preventing cervical cancer.(10,11,18,20,24)
When evaluating the
clinical skills of medical students, it was found that they had greater
knowledge about the etiopathology of cervical cancer and means of prevention,
compared to students from other health fields. In turn, obstetrics and nursing
students possessed greater knowledge about the technique and importance of
cytopathological examination and its purpose in screening for HPV and cervical
cancer.(24)
Thus, the impact of
health science training on the knowledge of university students is evident,
which was confirmed in a study conducted in Brazil with health science
students, as many of the participants acquired knowledge about cytopathological
examination through university and that its purpose is the screening of
cervical cancer. However, this same study identified that, despite knowing some
risk factors for the development of neoplasia, about half of the participants
did not consider HPV one of these factors; among these, half were nursing
students and had already taken the women's health course.(25)
This information is
alarming and demonstrates the need to evaluate and reformulate teaching in
undergraduate health science courses, seeking to provide efficient learning of
theoretical content, along with broad clinical practice that contributes to the
acquisition of the skills necessary to offer quality health care. Regarding
attitudes and practice, a limited number of investigations have explored these
dimensions. In investigations that addressed the attitude dimension, it was
observed that participants had favorable attitudes towards early detection
through cytopathological examination and intended to undergo the examination,(12,15,18)
believed there were effective methods for reducing the risk of cervical cancer,(15,18)
and recognized the need for the development of educational actions in the
university context.(20)
In this sense, it is
understood that the knowledge possessed by university students regarding the
severity of the neoplasm and the importance of prevention corroborates the
development of favorable attitudes that contribute to an effective change in
behavior, thus resulting in appropriate practice.
Regarding the
“practical” dimension, it was observed that female university students had a
low rate of adherence to cytopathological examination(15) and
vaccination.(9,10,16,18) The main factors cited as barriers to
vaccination were: lack of knowledge regarding the availability of the
immunobiological agent in the country, the price for administering the vaccine,
and concern about possible side effects.(16,24)
This review has
limitations in the number of databases searched, since relevant studies may not
have been included in the final sample, and the scarcity of studies developed
nationally on the knowledge, attitudes, and practices of female university students
regarding HPV and cervical cancer prevention.
It is worth highlighting that this review
will form the basis for the development of a KAP survey on HPV and cervical
cancer prevention among female university students, which may assist in the
development and implementation of health promotion policies, actions, and
strategies aimed at preventing HPV and cervical cancer. Understanding these
aspects is fundamental to identifying gaps in knowledge, cultural influences,
attitudes, and behavioral patterns that act as barriers to the implementation
of effective health interventions.
FINAL
CONSIDERATIONS
This study revealed that
female university students have adequate general knowledge about HPV and
cervical cancer, risk factors, transmission methods, and prevention and
screening methods. Furthermore, they held favorable attitudes towards early
detection through cytopathological examination and intended to undergo the
examination. Regarding practice, despite understanding the neoplasm as a fatal
disease, low rates of adherence to cytopathological examination and vaccination
were observed.
It was found that the
students have insufficient knowledge on topics such as symptoms, means of HPV
infection, diagnostic methods, and vaccination. Therefore, it is crucial that
more comprehensive and investigative educational strategies be implemented,
especially in the university context, to promote proactive attitudes and health
practices that minimize vulnerability to HPV and cervical cancer.
Thus, it is necessary
for healthcare professionals working in Primary Health Care to reinforce
strategies and actions aimed at primary and secondary prevention. Seeking to
achieve vaccination goals for the target population and reinforce the
importance of cervical cancer screening with cytopathological examination as a
complementary action in the prevention of neoplasia.
In addition, it is
essential that higher education institutions actively cooperate in the
development of educational actions for the prevention of HPV and cervical
cancer among their students and reformulate teaching in undergraduate health
courses, thus contributing to a comprehensive education aimed at quality
healthcare.
REFERENCES
1. Chilaka VN, Navti OB, Al Beloushi M, Ahmed B, Konje JC. Human
papillomavirus (HPV) in pregnancy – An update. Eur J Obstet Gynecol Reprod Biol
[Internet]. 2021;264:340-8. doi: https://doi.org/10.1016/j.ejogrb.2021.07.053.
2. Wild CP; Weiderpass E; Stewart BW, organizadores. World cancer
report: cancer research for cancer prevention. Lyon: International Agency for
Research on Cancer; 2020.
3. Bray F, Laversanne M, Sung H, Ferlay J, Siegel RL,
Soerjomataram I, et al. Global cancer statistics 2022: GLOBOCAN estimates of
incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J
Clin [Internet]. 2024;74(3):229-263. doi: https://doi.org/10.3322/caac.21834.
4. Brasil. Ministério da Saúde. Instituto Nacional de Câncer.
Estatísticas de câncer. Brasília (DF): INCA; 2023. Disponível em:
https://www.gov.br/inca/pt-br/assuntos/cancer/numeros.
5. Rashid S, Labani S, Das BC. Knowledge, Awareness and Attitude
on HPV, HPV Vaccine and Cervical Cancer among the College Students in India.
PLoS One [Internet]. 2016;11(11):e0166713. doi: https://doi.org/10.1371/journal.pone.0166713.
6. Alshammari F, Khan KU. Knowledge, attitudes and perceptions
regarding human papillomavirus among university students in Hail, Saudi Arabia.
Peer J [Internet]. 2022;10:e13140. doi: https://doi.org/10.7717/peerj.13140.
7. Merkuri L, Kamberi F, Qorri E, Shapo L. Assessment of the
Albanian University female students’ knowledge, attitudes, and practices on
cervical cancer. J Infect Dev Ctries [Internet]. 2023;17:534–541. doi: https://doi.org/10.3855/jidc.18121.
8. Mendes KDS, Silveira RCCP, Galvão CM. Uso de gerenciador de
referências bibliográficas na seleção dos estudos primários em revisão
integrativa. Texto Contexto Enferm [Internet]. 2019;28:e20170204. doi: https://doi.org/10.1590/1980-265X-TCE-2017-0204.
9. Pearson A, Jordan Z, McArthur A, Florescu S, Cooper A, Yan H,
Klugarova J, Stannard D, Edwards D. Systematic reviews of textual evidence:
narrative, expert opinion or policy. In: Aromataris E, Lockwood C, Porritt K,
Pilla B, Jordan Z, editores. JBI Manual for Evidence Synthesis. JBI; 2024. doi:
https://doi.org/10.46658/JBIMES-24-04.
10. Chen X, Xu T, Wu J, Sun C, Han X, Wang D, et al. Exploring
factors influencing awareness and knowledge of human papillomavirus in Chinese
college students: A cross-sectional study. Human Vaccines Immunotherapeutics
[Internet]. 2024;20(1):2388347. doi: https://doi.org/10.1080/21645515.2024.2388347.
11. Baptista AD, Simão CX, Santos VCG dos, Melgaço JG, Cavalcanti
SMB, Fonseca SC, et al.. Knowledge of human papillomavirus and Pap test among
Brazilian university students. Rev Assoc Med Bras [Internet].
2019;65(5):625–32. doi: https://doi.org/10.1590/1806-9282.65.5.625.
12. Binka C, Nyarko SH, Doku DT. Cervical Cancer Knowledge,
Perceptions and Screening Behaviour Among Female University Students in Ghana.
J Canc Educ. [Internet]. 2016;31:322–7. doi: https://doi.org/10.1007/s13187-015-0852-x.
13. Khan TM, Buksh MA, Rehman I U, Saleem A. Knowledge, attitudes,
and perception towards human papillomavirus among university students in
Pakistan. Papillomavirus Res [Internet]. 2016;2:122-7. doi: https://doi.org/10.1016/j.pvr.2016.06.001.
14. El Mansouri N, Ferrera L, Kharbach A, Achbani A, Kassidi F,
Rogua H, et al. Awareness and knowledge associated to Human papillomavirus
infection among university students in Morocco: A cross-sectional study. PLoS
One [Internet]. 2022;17(7):e0271222. doi: https://doi.org/10.1371/journal.pone.0271222.
15. Getaneh A, Tegene B, Belachew T. Knowledge, attitude and
practices on cervical cancer screening among undergraduate female students in
University of Gondar, Northwest Ethiopia: an institution based cross sectional
study. BMC Public Health. [Internet]. 2021;21:775. doi:
https://doi.org/10.1186/s12889-021-10853-2.
16. Widjaja VN. Awareness, Knowledge and Attitudes of Human
Papillomavirus (HPV) among Private University Students- Malaysia Perspective.
Asian Pac J Cancer Prev [Internet]. 2019;20(7):2045-50.
doi:10.31557/APJCP.2019.20.7.2045.
17. Mruts KB, Gebremariam TB. Knowledge and Perception Towards
Cervical Cancer among Female Debre Berhan University Students. Asian Pac J
Cancer Prev [Internet]. 2018;19(7):1771-77. doi: 10.22034/APJCP.2018.19.7.1771
18. Ndubuisi CC, Maphasha O, Okeke SO. Knowledge and awareness of
cervical cancer and human papillomavirus vaccination among female university
students. S Afr Fam Pract. [Internet]. 2024;66(1):a5885. doi: https://doi.org/10.4102/safp.v66i1.5885.
19. Koç, Z. University Students’ Knowledge and Attitudes Regarding
Cervical Cancer, Human Papillomavirus, and Human Papillomavirus Vaccines in
Turkey. J Am Coll Health [Internet]. 2014;63(1):13–22. doi: https://doi.org/10.1080/07448481.2014.963107.
20. Balaji M, Panwar A, Kudva MA, Ballal NV, Keluskar V. Awareness
and Knowledge Among Dental and Medical Undergraduate Students Regarding Human
Papilloma Virus and Its Available Preventive Measures. Ann Glob Health
[Internet]. 2020;86(1):150. doi: 10.5334/aogh.2826.
21. Divya KT, Chidrawar VR, Bhupalam PK, Shiromwar S, Aljameeli
AM, Vyshnavi G, et al. Assessment of knowledge and attitude of cervical cancer
among the youths in the Rayalaseema region of Andhra Pradesh–India. J Educ
Health Promot [Internet]. 2024;13(1):73. doi:10.4103/jehp.jehp_318_23.
22. Al-Shaikh GK, Almussaed EM, Fayed AA, Khan FH, Syed SB,
Al-Tamimi TN, et al. Knowledge of Saudi female university students regarding
cervical cancer and acceptance of the human papilloma virus vaccine. Saudi Med
J [Internet]. 2014;35(10):1223-30. Disponível em: https://pmc.ncbi.nlm.nih.gov/articles/PMC4362125/pdf/SaudiMedJ-35-1223.pdf.
23. Yilmazel G, Duman NB. Knowledge, attitudes and beliefs about
cervical cancer and human papilloma virus vaccination with related factors in
Turkish university students. Asian Pac J Cancer Prev. [Internet].
2014;15(8):3699-704. doi: https://doi.org/10.7314/APJCP.2014.15.8.3699.
24. Yörük S, Açıkgöz A, Ergör G. Determination of knowledge
levels, attitude and behaviors of female university students concerning
cervical cancer, human papiloma virus and its vaccine. BMC Womens Health
[Internet]. 2016;16:51. doi: https://doi.org/10.1186/s12905-016-0330-6.
25. Lima CAD, Amaral JG, Oliveira PPD, Santos WJD, Rodrigues AB,
Aguiar MIFD. Câncer do colo de útero: conhecimento de estudantes
universitários. Rev. enferm. UFPE on line [Internet]. 2016;10(8):2993-3003.
doi: 10.5205/reuol.9373-82134-1-RV1008201626.
Funding and
Acknowledgments:
This research
received no funding.
Data
Availability Statement No databases were
generated in this study. The information presented is described in the body of
the article.
Authorship
Criteria (Author Contributions)
Authorship
designation should be based on ICMJE guidelines, which consider an author to be
someone who: 1. contributes substantially to the conception and/or planning of
the study; 2. to the acquisition, analysis, and/or interpretation of the data;
3. as well as to the drafting and/or critical revision and final approval of
the published version.
Rawane Soares
Santos 1 2 3
José Cláudio
Garcia Lira Neto 1 3
Jardeliny
Corrêa da Penha 3
José Ribamar
Lopes Batista Júnior 3
Maria Augusta
Rocha Bezerra 3
Conflict of
Interest Statement
Nothing to
declare.
Scientific
Editor: Ítalo Arão Pereira Ribeiro. Orcid:
https://orcid.org/0000-0003-0778-1447
Rev Enferm Atual
In Derme 2026;100(1): e026033

