CASE STUDY
SURGICAL DEHISCENCE IN ABDOMINOPLASTY: THE USE OF DIALKYL CARBAMOYL CHLORIDE IN THE HEALING PROCESS
DEISCÊNCIA OPERATÓRIA EM ABDOMINOPLASTIA: O USO DE CLORETO DE DIALQUIL CARBAMOIL NO PROCESSO DE CICATRIZAÇÃO
DEHISCENCIA OPERATORIA EN ABDOMINOPLASTIA: EL USO DE CLORURO DE DIALQUIL CARBAMOILO EN EL PROCESO DE CICATRIZACIÓN
https://doi.org/10.31011/reaid-2026-v.100-n.2-art.2664
1Luanna Dias de Assis
2Ana Paula Martins Casagrande
3Heloísa Helena Camponez Bárbara Rédua
4Lucas Dalvi Armond Rezende
5Natalia Aparecida de Barros
6Paula de Souza Silva Freitas
1Enfermeira - Universidade Federal do Espírito Santo. Vitória - ES, Brazil - https://orcid.org/0009-0007-6167-8797
2Enfermeira especialista em enfermagem dermatológica - Consultório privado de prática avançada no tratamento de feridas operatórias. Vitória - ES, Brazil - https://orcid.org/0009-0000-0194-1441
3Enfermeira e Estomaterapeuta - Universidade Federal do Espírito Santo. Vitória - ES, Brazil - https://orcid.org/0009-0007-8311-7296
4Enfermeiro especialista em Oncologia. Mestrando em medicina pela UFRJ - Universidade Federal do Rio de Janeiro. Professor Associado do Colegiado de Enfermagem do Centro Universitário Salesiano. Vitória - ES, Brazil - https://orcid.org/0000-0002-3313-852X
5Enfermeira estomaterapeuta, com aperfeiçoamento em dermatologia em enfermagem, MBA em gestão de mkt - Essity Brazil. São Paulo - SP, Brazil - https://orcid.org/0009- 0006-5917-6619
6Enfermeira e Professora da Universidade Federal do Espírito Santo - Universidade Federal do Espírito Santo. Vitória - ES, Brazil - https://orcid.org/0000-0001-9066-3286
Corresponding Author
Paula de Souza Silva Freitas
Avenida São Paulo, nº 2760, ap 803, Edifício Costa Azurra, Itapoã, Vila Velha - ES, Brazil. CEP: 29101502, contact: +5527993167281, E-mail¨paulassfreitas@gmail.com.
Submission: 07-10-2025
Approval: 20-03-2026
RESUMO
Introdução: A cirurgia plástica estética tem como finalidade a melhoria da aparência e da autoestima. Entre os procedimentos cirúrgicos, a deiscência de ferida operatória se destaca como uma complicação relevante, pois está associada ao prolongamento do tratamento, ao aumento dos custos e ao comprometimento da qualidade de vida do paciente. Para o êxito no seu manejo, é fundamental a adoção de práticas baseadas em evidências. Objetivo: Avaliar a evolução de uma deiscência de ferida operatória com o uso de curativo antimicrobiano revestido com cloreto de dialquil carbamoil. Método: Trata-se de um relato de caso sobre o tratamento de deiscência de ferida operatória em uma paciente, submetida à abdominoplastia, em um consultório localizado em um município do Espírito Santo, entre dezembro de 2023 e março de 2024, por meio do prontuário eletrônico e de entrevista. Resultados: Paciente do sexo feminino, 43 anos, parda, sem comorbidades, com deiscência de ferida operatória que apresentava as seguintes características: bolhas e sinais de hipóxia tecidual em região perilesional. A ferida apresentava as seguintes proporções: 15 cm de comprimento e 1,5 de largura. A partir do terceiro atendimento foi utilizado curativo antimicrobiano impregnado com cloreto de dialquil carbamoil. Ao final de 3 meses de tratamento, a lesão evoluiu para cicatrização completa. Considerações finais: Foi observado que após a utilização da cobertura antimicrobiana, juntamente com a aplicação do protocolo de limpeza da ferida, houve melhoria no processo de cicatrização da ferida. Ressalta-se também a discrepância entre as melhores evidências e as condutas profissionais.
Palavras-chave: Deiscência da Ferida Operatória; Cuidados de Enfermagem; Cicatrização.
ABSTRACT
Introduction: Aesthetic plastic surgery aims to improve appearance and self-esteem. Among surgical procedures, wound dehiscence stands out as a significant complication, as it is associated with prolonged treatment, increased costs, and impaired patient quality of life. For successful management, the adoption of evidence-based practices is essential. Objective: To evaluate the progression of wound dehiscence with the use of an antimicrobial dressing coated with dialkyl carbamoyl chloride. Method: This is a case report on the treatment of wound dehiscence in a patient undergoing abdominoplasty in a clinic located in a city in Espírito Santo, between December 2023 and March 2024, using electronic medical records and interviews. Results: A 43-year-old female patient, brown skin color, without comorbidities, presented with surgical wound dehiscence that presented the following characteristics: blisters and signs of tissue hypoxia in the perilesional region. The wound measured 15 cm long and 1.5 cm wide. From the third visit onward, an antimicrobial dressing impregnated with dialkyl carbamoyl chloride was used. After 3 months of treatment, the wound healed completely. Final considerations: It was observed that after the use of antimicrobial dressing, together with the application of the wound cleaning protocol, there was an improvement in the wound healing process. The discrepancy between the best evidence and professional practices is also noteworthy.
Palavras-chave: Surgical Wound Dehiscence; Nursing Care; Wound Healing.
RESUMEN
Introducción: La cirugía plástica estética tiene como objetivo mejorar la apariencia y la autoestima. Entre los procedimientos quirúrgicos, la dehiscencia de la herida se destaca como una complicación significativa, ya que se asocia con un tratamiento prolongado, mayores costos y deterioro de la calidad de vida del paciente. Para un manejo exitoso, la adopción de prácticas basadas en la evidencia es esencial. Objetivo: Evaluar la progresión de la dehiscencia de la herida con el uso de un apósito antimicrobiano recubierto con cloruro de dialquil carbamoilo. Método: Se trata de un informe de caso sobre el tratamiento de la dehiscencia de la herida en un paciente sometido a abdominoplastia en una clínica ubicada en una ciudad de Espírito Santo, entre diciembre de 2023 y marzo de 2024, mediante historias clínicas electrónicas y entrevistas. Resultados: Una paciente de 43 años, de piel morena, sin comorbilidades, presentó dehiscencia de la herida quirúrgica que presentó las siguientes características: ampollas y signos de hipoxia tisular en la región perilesional. La herida medía 15 cm de largo y 1,5 cm de ancho. A partir de la tercera visita, se utilizó un apósito antimicrobiano impregnado con cloruro de dialquil carbamoilo. Tras 3 meses de tratamiento, la herida sanó completamente. Consideraciones finales: Se observó una mejoría en la cicatrización tras el uso del apósito antimicrobiano, junto con la aplicación del protocolo de limpieza de heridas. Cabe destacar la discrepancia entre la mejor evidencia y las prácticas profesionales.
Palavras-chave: Dehiscencia de la Herida Operatoria; Atención de Enfermería; Cicatrización de Heridas.
INTRODUCTION
The Brazilian Society of Plastic Surgery (SBCP) conceptualizes plastic surgery as a surgical specialty dedicated to the reconstruction of body structures that present morphological or functional alterations, resulting from congenital or acquired deformities. When it comes to aesthetic plastic surgery, which has become increasingly popular worldwide, it aims to improve the appearance and self-esteem of people and whose cause is not necessarily related to health issues or deformities(1). According to the International Society of Aesthetic Plastic Surgery, in 2023, Brazil ranked second in the number of procedures performed worldwide, totaling 3.3 million, and first in surgical procedures, with 2.1 million(2).
Since it is a surgical procedure, its practice presents complication risks, including surgical wound dehiscence (SWD), defined as the separation of the margins of a closed surgical incision that may or may not involve infection.(3). Dehiscence may be due to: surgical technique, infection, mechanical stress (like coughing, vomiting, and abrupt or vigorous movement), presence of hematoma or seroma, and factors related to the patient’s clinical condition (such as diabetes, hypertension, obesity, smoking, previous surgery on the same site of incision, and immunodepression)(3).
Additionally, one study concluded that infected SWD are double the cost of non-infected wounds. Thus, it is perceptible that this complication causes economic impacts, in addition to increasing treatment time and interfering with the quality of life of patients(4). Regarding surgical wound infections, one of the main challenges is managing the biofilm, an extracellular polymeric matrix composed of polysaccharides, proteins, extracellular DNA, and metal-binding ions that form a physical barrier to the community of microorganisms within it. This impairs access to antimicrobial agents and immune system cells, promoting chronic inflammation and increased risk of antimicrobial resistance. Thus, biofilm must not be treated the same way as acute infections(5).
Regarding treatment, it must be guided by evidence-based practices, whose objective is to combine the best scientific evidence and clinical practice, therefore enabling improved quality of the provided care to reduce risks and errors(6). The treatment of SWD, when there are signs of biofilm, involves wound hygiene and the use of antiseptics, together with antimicrobial dressings, which help control the bacterial load and promote healing(7).
In this sense, this case report aims to describe the evolution of a surgical wound dehiscence after abdominoplasty, reinforcing the importance of choosing appropriate dressings for its treatment through an evidence-based care plan.
METHODS
This is a case report on the treatment of surgical wound dehiscence using dialkyl carbamoyl chloride (DACC) on a patient submitted to abdominoplasty with liposculpture at a medical practice located in a city in Espírito Santo. A dermatological nurse conducted the consultations. The patient follow-up was conducted between December 2023 and March 2024, totaling 8 in-person sessions. Complementary data was obtained through electronic medical records and interviews. The TIMERS tool by the Journal Wound Care International Consensus(8) was used to assess the wound. A Free and Informed Consent Form was applied, which also contained permission to use the images showing wound evolution. This study has been approved by the Research Ethics Committee, report number 7,729,844.
RESULTS
After initiating treatment with DACC, the wound evolved to close completely with epithelialization tissue in 67 days, as reported next:
Clinical case
A 43-year-old female patient, nurse, brown skin color, without comorbidities, with a previous history of C-section, does not use medication on a continuous basis, living with 2 children and her husband in Santa Leopoldina. Has a BMI of 24.27 kg/m². Underwent total abdominoplasty with liposculpture on November 29, 2023, and upon hospital discharge (3 days after surgery) was diagnosed with epitheliosis, characterized by low blood perfusion in the wounded area.
At first, the surgical wound presented a blackened region with the presence of blisters in a perilesional area, indicating tissue hypoxia, with a risk of necrosis (Figure 1). Thus, a neomycin sulfate 5 mg/g + zinc bacitracin 250 Iu/g ointment, prescribed by the surgeon, was applied. During the same period, the patient sought help from the nurse, who advised her not to use the topical antibiotic because it is contraindicated for wound treatment based on the best available evidence. Thus, both the nurse and the doctor guided the patient to undergo high-pressure, or hyperbaric, oxygen therapy, but she did not do it as the service was not available where she lives, and she was not available to travel to the cities where this treatment was possible.
Therefore, the patient opted to follow the medical advice, even though the nurse advised her not to use the ointment. Then, after 12 days of using the ointment, there was wound bed exposure, with presentation of necrotic tissue in almost all the wound extension (Figure 2), and the patient was guided by the surgeon to wash the wound in the shower and apply collagenase with chloramphenicol. However, there was no clinical evolution, and the wound bed presented increased necrotic tissue and crumbling (Figure 3).
Thus, 28 days after showing signs of dehiscence and employing the aforementioned treatment, with no signs of improvement, the patient opted to follow wound treatment with the dermatological nurse.
Figure 1 - Surgical wound 3 days after the surgery (Dec. 02, 2023).
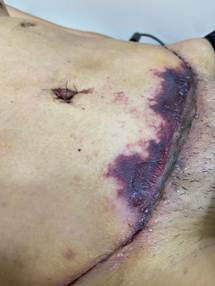
Source: authors’ personal archive.
Caption: surgical wound with signs of tissue hypoxia.
Figure 2 - Wound after using topical antibiotic (Dec. 14, 2023).
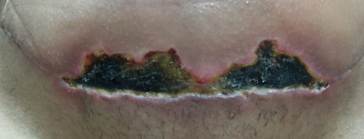
Source: authors’ personal archive.
Caption: Dehiscence with bed fully covered by inviable tissue, elevated margins, maceration in the lower portion of the margin, and perilesional erythema.
Figure 3 - Wound after using collagenase with chloramphenicol (Dec. 22, 2023).
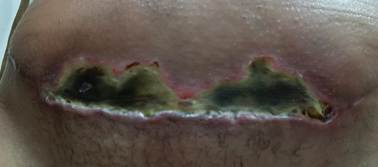
Source: authors’ personal archive.
Caption: Dehiscence with bed fully covered by inviable tissue, elevated margins, maceration in the lower portion of the margin, and perilesional erythema.
Evolution of the wound
On the first consultation, the wound (Figure 4) was characterized as grade 2a, based on the World Union of Wound Healing Societies 2018 classification of Surgical Wound Dehiscence, presenting adipose tissue exposure, crumbling in the wound bed, elevated and macerated margins, hyperemia in the perilesional area, and a great volume of serous exudate. The wound measured 15 cm long and 1.5 cm wide. Instrumental debridement was performed, the wound was cleaned with a polyhexamethylene biguanide (PHMB) solution, hydrofiber was applied as a primary dressing, an antimicrobial gauze compress impregnated with PHMB was applied as a secondary dressing, and the wound was occluded with a transparent polyurethane film. Additionally, the patient was advised to protect the wound when showering and change the primary and secondary dressings every 2 days, a practice that was virtually followed up by sending pictures to the nurse at every dressing change.
Figure 4 - Dehiscence on Dec. 12, 2023.
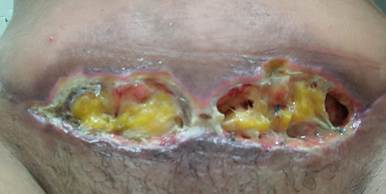
Source: authors’ personal archive.
Caption: dehiscence with exposure of adipose tissue, presenting inviable tissue, elevated margins, maceration in the lower portion of the margin, and perilesional erythema.
Before the second consultation, the surgeon approached to perform wound debridement. Therefore, on this consultation, the wound presented clinical improvement (figure 5). Presents granulation tissue, exposure of adipose tissue, presence of adhered crumbling, and elevated margins. The exudate remained serous in great volume. The conduct was to perform instrumental debridement and clean the wound with a PHMB solution. Hydrofiber was used as a primary dressing, and an antimicrobial gauze compress impregnated with PHMB as secondary dressing, and the wound was occluded with a transparent polyurethane film. Moreover, the patient kept changing the dressing every 2 days with virtual follow-up.
Figure 5 - Dehiscence on Jan. 05, 2024.
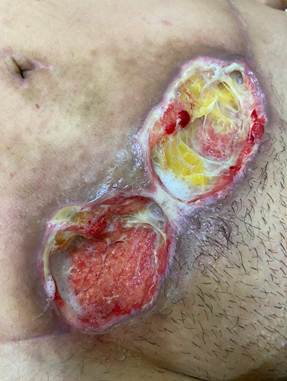
Source: authors’ personal archive.
Caption: cavitary dehiscence with exposure of adipose tissue, bed with granulation tissue, little volume of inviable tissue, and elevated margins.
In the third consultation, the wound (Figure 6) kept the presence of granulation tissue, exposure of adipose tissue, and adhered crumbling. There was decreased exudate, which remained serous, and margins with epibole.
The conduct was to perform instrumental debridement followed by wound cleaning with a PHMB solution, margin exacerbation, and application of 9J photodynamic therapy with methylene blue onto the wound bed. Aiming to keep fighting the infection and biofilm, and in the face of the chemical substance use duration, PHMB, and respecting the recommendation of antimicrobial rotation, the team decided to initiate treatment with a dressing coated in a physical antimicrobial, an acetate screen coated with dialkyl carbamoyl chloride as a primary dressing. The antimicrobial gauze compress impregnated with PHMB at 0.2% was kept as a secondary dressing, and the wound remained occluded with a transparent polyurethane film.
Figure 6 - Dehiscence on Jan. 12, 2024.
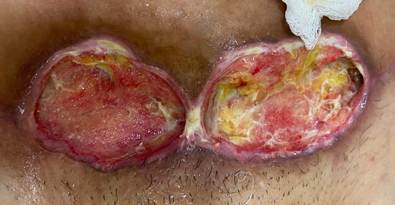
Source: authors’ personal archive.
Caption: cavitary dehiscence with exposure of adipose tissue, bed with granulation tissue, little volume of inviable tissue, and margins in epibole.
The conduct from consultations 4, 5, and 6 (Jan. 23, 2024 - Jan. 30, 2024 - Feb. 05, 2024) was kept according to consultation 3, considering there was no clinical aggravation.
In consultation 7, the wound (Figure 7) presented with granulation tissue and epithelialization areas, with flat and irregular margins.
The conduct was to clean the wound with PHMB solution, perform red 2J photobiomodulation therapy on the wound bed, use an acetate screen coated with DACC as primary dressing, an antimicrobial gauze impregnated with 0.2% PHMB as secondary dressing, and occlude it with transparent polyurethane film.
Figure 7 - Dehiscence on Feb. 14, 2024.
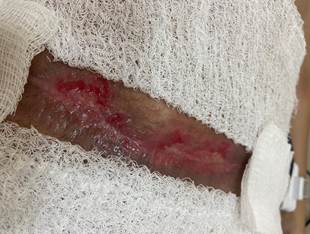
Source: authors’ personal archive.
Caption: dehiscence with the presence of epithelialization tissue and granulation tissue, and flat and irregular margins.
Between consultations 7 and 8, the patient could not be physically present, so the wound cleaning and dressing change were performed by the patient herself in her home, virtually followed up by the nurse. During that period, the following routines were maintained: cleaning with PHMB, using an acetate screen coated in DACC as primary dressing, antimicrobial gauze compress impregnated with 0.2% PHMB as secondary dressing, and occlusion with transparent polyurethane film. Thus, in consultation 8, the wound already presented complete healing (Figure 8). Due to the clinical case improvement, the patient was discharged and advised on how to care for the scarred region.
Figure 8 - Evolution of the wound, finishing with total epithelialization on Mar. 19, 2024.
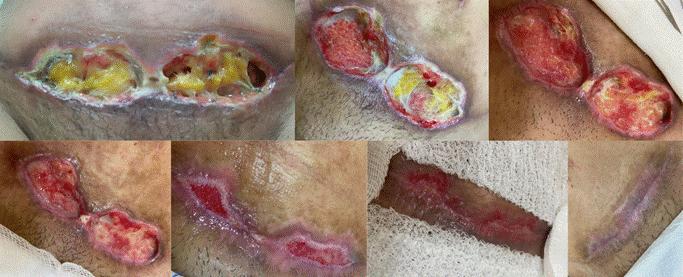
Source: authors’ personal archive.
DISCUSSION
By analyzing the development of the dehiscence, it can be stated that this is a difficult-to-heal wound, since there is stagnation in this process due to the presence of biofilm.(7). Studies in the area of wound treatment suggest that biofilms tend to form more easily in wounds that present an excess of exudate and inviable tissue, as in the discussed case. This happens because this kind of environment offers ideal conditions for the proliferation of microorganisms, since there is constant humidity and nutrients available(9).
Despite the patient in the described case having no comorbidities, she presents tissue hypoxia in the surgical wound area (Figure 1), which is a local risk factor for dehiscence and a difficulty factor for healing(4). Although there is no detailing in the literature of this pathology in the surgical area and recommended therapies, given the physiological plausibility, it is possible to consider high-pressure or hyperbaric oxygen therapy as an intervention for the presented tissue hypoxia, since it works by increasing the partial pressure on these tissues to suppress metabolic needs and enable healing(10). However, the distance from the patient’s residence to the cities where this service is offered made the use of hyperbaric oxygen therapy impossible.
Given the presented complication, the medical professional’s approach was to prescribe a topical antibiotic, which is not in line with best practices as it does not eradicate the biofilm, only kills the microorganisms that help prepare the immunologic cells for the healing process, and can cause antimicrobial resistance. Thus, the evidence contraindicates the general use of topical antibiotics for managing infection in wounds(5,9).
Another approach that diverges from the scientific evidence is the prescription of collagenase with chloramphenicol, since the product’s objective is enzymatic debridement, being recommended for inviable tissue removal in non-exudative wounds(11-12), in addition to containing chloramphenicol, a topical antibiotic not recommended by the best evidence for the treatment of local wound infection(9).
Moreover, regarding the recommendation to wash the wound in the shower, a recent systematic review found no difference in surgical wound infection when comparing patients who wet their wound in the shower within 48 hours of surgery with patients who wet their wound in the shower 48 hours after the surgery. However, that study did not compare patients who exposed the wound in the shower to those who did not expose it; thus, it is not possible to state that there is no risk of infection. The result of that research may encourage the practice of washing the wound in the shower, even though authors highlight that there must be bathroom disinfection and water quality control, which is not feasible in a country as unequal as Brazil(13). Under this perspective, this practice increases the risk of infection as water carries microorganisms from other regions of the body into the wound bed. Therefore, this guidance is contraindicated as it offers risks to the patient’s health. The best practice advises the use of waterproof dressings in surgical wounds until their complete epithelialization(7).
Drinking water may be used only in situations in which no other resources are available to clean the wound, which may be read as validation to some people. However, evidence advises not to use stagnant water and boil it before use, a situation in which there is still risk of infection. Additionally, the use of saline solution or sterilized water is recommended, with saline solution being preferred for being isotonic and not disturbing the wound bed. Moreover, the wound cleaning technique involves applying a continuous flow of solution in the pressure range of 8 to 15 pounds per inch square to remove debris and microbes from the wound without compromising tissue integrity, which does not happen when the wound is washed during the shower(14).
Regarding the dressings used, the nurse who managed the surgical wound dehiscence chose hydrofiber plaque in the consultations before January 12 because the wound had excessive exudate. Hydrofiber has a high absorption capacity, decreasing the risk of maceration. Additionally, when in contact with the exudate, the plaque forms a gel that keeps the wound bed humid, aiding in healing and performing safe autolytic debridement(15).
According to best practices, the International Consensus on Surgical Wound Hygiene provides that surgical wounds with dehiscence must follow 4 steps: Cleaning, debridement, remodeling, and application of dressing(7).
In the cleaning step of wounds with clinical signs of biofilm, as the present case, the International Wound Infection Institute (IWII) best practices consensus recommends using low cytotoxicity antiseptics, like PHMB, for instance, along with debridement and antimicrobial dressings, as they have antibiofilm action. But they suggest its use be considered only in situations with a risk of infection, presence of infection, and existence of biofilm(5,14).
The DACC-coated acetate screen chosen in the fourth step of wound hygiene converges with the scientific evidence, given that it is a non-medicated dressing, that is, it has no active bactericide or bacteriostatic component. This dressing has a technology that physically acts on microorganisms, irreversibly fixing on their extracellular surface through hydrophobic connections. Thus, it has no risk of antimicrobial resistance, in addition to being safe for prolonged use on wounds(5,16).
Figure 9 - DACC-coated acetate screen applied to the wound bed.

Source: authors’ personal archive.
Regarding adjuvant therapies, low-level laser therapy (LLLT) was used, which significantly contributes to pain and inflammation management, in addition to favoring synthesis and cell proliferation, like fibroblasts and keratinocytes, in the healing process, and increased vascularization, contributing to epithelialization(17-18).
During consultations 3, 4, and 5, Photodynamic Therapy (PDT) was employed with a bactericidal goal. The mechanism of action of this therapeutic practice is based on the combination of three non-toxic components: one photosensitizer (in this case, methylene blue), oxygen, and 600 nm wavelength light, at a dose of 9 Joules and irradiation duration of 90 seconds per spot in the wound bed. The interaction between these elements generates oxidative stress capable of damaging essential components of microbial cells and, consequently, causing the death of previously stained pathogenic cells(19).
Although most studies related to the application of PDT have been conducted in in vitro and non-human in vivo models, there is a randomized clinical trial showing a better outcome in patients who have been submitted to photodynamic therapy when compared to those who did not receive this treatment, with decreased wound and microbial load. Therefore, such conduct seems to be effective in the treatment of wounds infected with microorganisms and with the presence of biofilm(20-22).
Figure 10 - Application of photodynamic therapy
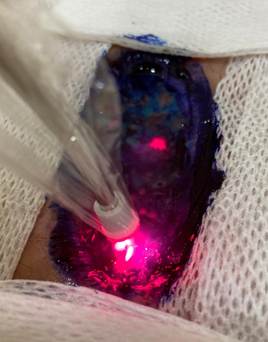
Source: authors’ personal archive.
Caption: Wound bed stained with methylene blue at 1% concentration and 9 Joules red light irradiation.
Regarding the challenges of interprofessional work, given the fact that the patient followed the doctor’s orientation, even after receiving guidance from the nurse, and the delay in following nursing practices, a study conducted with users of Municipal Health Center showed that most patients believed nurses are subordinate to medical professionals. It is possible, therefore, to relate the preference of following the doctor’s orientation with a history of invisibility of the nursing work, which causes low social recognition in a doctor-centered health scenario(23).
Under this perspective, interprofessionalism and dialog between professional categories should be highlighted as a challenge in surgical wound management. There must be communication between the professionals working in surgery and those working in surgical wound management so that the process of care is standardized and promotes an effective outcome in the treatment of SWDs. Therefore, professionals must acknowledge their legal limits and refer patients who did not have at least 40% reduction in the wounded area in 4 weeks of treatment to an evaluation with specialists, such as stoma therapists or dermatological nurses(7-8).
Given this scenario, the specialist nurse plays a fundamental role in SWD prevention and treatment. In the pre-surgical and intrasurgical period, their attributions include assessing the risk of infection and dehiscence, verifying adherence to aseptic techniques in every step — from skin preparation to the adequate glove change when closing the surgical wound — and adopting measures for preventing hypothermia during surgery. In the postoperative period, we highlight the responsibility for elaborating educational plans targeted at patient self-care, including guidance on wound and drain management, preventing mechanical complications, and wound care. Health education must also contemplate protection strategies during movements that employ too much effort, such as coughing and mobilization, contributing to reducing the risk of SWD. Therefore, it is extremely important to have the follow-up of a specialist nurse in the pre-, intra-, and postoperative periods to assess the risk of complications, prevent them, and treat them, if needed. Studies suggest this measure decreases the risk of unfavorable outcomes, like surgical wound dehiscence(24-25).
FINAL CONSIDERATIONS
The case unveiled in this study showed improvement in the healing process of dehiscence with biofilm after applying the surgical wound hygiene protocol along with non-medicated antimicrobial dressings, and reinforces the need for dialog between healthcare professionals within the multiprofessional team. It also demonstrates the discrepancy between the best evidence and professional practices. Thus, it is imperative that professional training invests in evidence-based practices as the foundation of professional conduct in the treatment of surgical wounds.
It is also necessary to involve the patient in their own process of care, preparing them to identify signs in their surgical wound and be ready to seek health assistance.
Furthermore, a gap was observed in studies regarding wound care related to tissue hypoxia in surgical wounds, especially concerning the risk factors for this condition and the recommended treatment.
REFERENCES
- Lima DSC. et al. A cirurgia plástica na mídia: o conceito da especialidade veiculado pelos meios de comunicação impressos no Brasil. Rev Bras Cirurgia Plástica. jan.–mar. 2015;30(1). DOI:10.5935/2177-1235.2015RBCP0122
- International Society of Aesthetic Plastic Surgery. Global Survey 2023: full report and press releases. Mount Royal, NJ: ISAPS; 12 jun. 2024. Disponível em: https://www.isaps.org/discover/about-isaps/global-statistics/global-survey-2023-full-report-and-press-releases/.
- Sandy‑hodgetts K et al. Surgical wound dehiscence (SWD): International consensus statement on assessment, diagnosis and management. London: Wounds International, 2023. 23 p. Disponível em: https://woundsinternational.com/wp-content/uploads/2024/06/SN24_CD_SWD_WINT_WEB.pdf.
- Sandy‑hodgetts K et al. Optimising prevention of surgical wound complications: detection, diagnosis and prediction. Londres: Wounds International; 2022. Disponível em: https://woundsinternational.com/wp-content/uploads/2023/02/933dfca2e2e9ea57418b7fe1e165d9e0.pdf
- World Union of Wound Healing Societies. The role of non-medicated dressings for the management of wound infection. London: Wounds International; 2020. Disponível em: https://woundsinternational.com/wp-content/uploads/2023/02/a1ad1513beed2c83e05f823ce5c977d8.pdf.
- Ferraz L et al. Ensino e aprendizagem da prática baseada em evidências nos cursos de Enfermagem e Medicina. Rev Bras Estudos Pedagógicos. 18 jun. 2019;101(257). DOI: https://doi.org/10.24109/2176-6681.rbep.101i257.4424.
- Murphy C et al. A proactive healing strategy for tackling biofilm-based surgical site complications: Wound Hygiene Surgical. J Wound Care. 1 maio 2024; 33(Suppl5a): S1–S30. DOI: 10.12968/jowc.2024.33.Sup5c.S1. Disponível em: https://www.magonlinelibrary.com/doi/pdf/10.12968/jowc.2024.33.Sup5c.S1.
- Atkin L et al. Implementing TIMERS: the race against hard-to-heal wounds. Londres: Journal of Wound Care. 2019;28(Suppl.3a): S1–S50. doi: 10.12968/jowc.2019.28.Sup3a.S1. Disponível em: https://www.magonlinelibrary.com/doi/pdf/10.12968/jowc.2019.28.Sup3a.S1.
- International Wound Infection Institute. Wound infection in clinical practice: principles of best practice. Londres: Wounds International; 2022. Disponível em: https://woundinfection-institute.com/wp-content/uploads/IWII-CD-2022-web-1.pdf.
- Barbosa PRA et al. Oxigenoterapia hiperbárica no processo de cicatrização de feridas: revisão de literatura. Rev Enfermagem Atual In Derme. jul./set. 2020;93(31): e‑020031. Disponível em: https://revistaenfermagematual.com.br/index.php/revista/article/view/610.
- Sociedade Brasileira de Estomaterapia. Preparo do leito da lesão. São Paulo: SOBEST; URGO. 2016. Disponível em: https://sobest.com.br/wp-content/uploads/2020/10/Preparo-do-leito-da-ferida_SOBEST-e-URGO-2016.pdf.
- Mayer DO et al. Best practice for wound debridement: international consensus document. Londres: Journal of Wound Care. 2024;33(suppl. 6): S1–S17. Disponível em: https://www.journalofwoundcare.com/docs/debridement-consensus.pdf.
- Ren Yu, Yu Hui, Wang Z, Pan W, Chen L, Luo H. Does earlier bathing increase the risk of surgical site infection? A meta-analysis of 11 randomized controlled trials. EFORT Open Reviews. 3 jun. 2024;9(6): 458–66. DOI: 10.1530/EOR-23-0062. PMCID: PMC11195341.
- International Wound Infection Institute. Therapeutic wound and skin cleansing: clinical evidence and recommendations. Londres: Wounds International; 2025. Disponível em: https://sobest.com.br/wp-content/uploads/2025/05/Therapeutic-wound-and-skin-cleansing.pdf.
- Weller CD et al. First-Line Interactive Wound Dressing Update: A Comprehensive Review of the Evidence. Frontiers in Pharmacology. 28 fev. 2020; 11:15. DOI: 10.3389/fphar.2020.00155
- Freitas PSS et al. Utilização do cloreto de dialquil carbamoil na prevenção e tratamento de biofilme em feridas. Estima, Braz J Enterostomal Therapy. 2021;19: e1621. Disponível em: https://www.revistaestima.com.br/estima/article/view/1087/464.
- Blascovich HB, Nogueira AG, Jesus Costa ACP. Parâmetros e protocolos da laserterapia utilizados no tratamento de feridas diabéticas. Rev Enfermagem Atual In Derme. 12 abr. 2022;96(38). DOI: 10.31011/reaid-2022-v.96-n.38-art.1321. Disponível em: https://revistaenfermagematual.com.br/index.php/revista/article/view/132.
- Tamimi R et al. Review on the molecular mechanisms of low-level laser therapy: gene expression and signaling pathways. Lasers in Medical Science. 2025; 40(160). DOI: 10.1007/s10103-025-04393-z.
- Wang L, Chen Q, Liu D. Development of Photodynamic Therapy in Treating Oral Diseases. Frontiers in Oral Health. 15 jan. 2025;5. DOI: 10.3389/froh.2024.1506407.
- Bernardes LO, Jurado SR. Efeitos da laserterapia no tratamento de lesões por pressão: uma revisão sistemática. Colombia: Rev Cuidarte. 2018; 9(3): 2423–34. DOI: https://doi.org/10.15649/cuidarte.v9i3.574. Disponível em: https://revistas.udes.edu.co/cuidarte/article/view/574.
- Li J et al. Fungicidal efficacy of photodynamic therapy using methylene blue against Sporothrix globosa in vitro and in vivo. European J Dermatol. 2019;29(2): 160–66. DOI: 10.1684/ejd.2019.3527.
- Brandão MGSA, et al. Antimicrobial photodynamic therapy in the treatment of foot ulcers in people with diabetes mellitus: a randomised controlled trial protocol. WCET® Journal. 2024;44(4):28-38. DOI 10.33235/wcet.44.4.28-38.
- Ribeiro, DFS et al. A identidade profissional da enfermeira na percepção de usuários da Atenção Básica. Rev Bras Enfermagem. 2022; 75(3): e20200974. DOI: 10.1590/0034-7167-2020-0974.
- Bashaw MA, Keister KJ. Perioperative strategies for surgical site infection prevention. AORN Journal. jan. 2019;109(1): 68–78. DOI: 10.1002/aorn.12451.
- Gomes ET, Poveda VB, Püschel VAA. Ações de enfermagem podem prevenir deiscência em ferida operatória? Rev SOBECC. abr./jun. 2020;25(2): 114–19. DOI: 10.5327/Z1414‑4425202000020008. Disponível em: https://revista.sobecc.org.br/sobecc/article/view/553.
Funding and Acknowledgments:
No funding received.
Conflict of Interest Statement:
Nothing to declare.
Data Availability Statement:
No databases were generated in this study. The information presented is described in the body of the article.
Author Contributions:
Luanna Dias de Assis: Conceptualization, Data Curation, Formal Analysis, Investigation, Methodology, Visualization, Original Draft Writing, Writing - Revision and Editing.
Ana Paula Martins Casagrande: Conceptualization, Data Curation, Formal Analysis, Investigation, Methodology, Visualization, Original Draft Writing, Writing - Revision and Editing.
Heloísa Helena Camponez Bárbara Rédua: Conceptualization, Data Curation, Formal Analysis, Investigation, Methodology, Visualization, Original Draft Writing, Writing - Revision and Editing, Supervision.
Lucas Dalvi Armond Rezende: Conceptualization, Data Curation, Formal Analysis, Investigation, Methodology, Visualization, Draft Writing, Original Writing, Writing - Revision and Editing, Supervision.
Natalia Aparecida de Barros: Conceptualization, Data Curation, Formal Analysis, Investigation, Methodology, Visualization, Draft Writing, Original Writing, Writing - Revision and Editing.
Paula de Souza Silva Freitas: Conceptualization, Data Curation, Formal Analysis, Investigation, Methodology, Visualization, Draft Writing, Original Writing, Writing - Revision.
Scientific Editor: Ítalo Arão Pereira Ribeiro. Orcid: https://orcid.org/0000-0003-0778-1447
Rev Enferm Atual In Derme 2026;100(2): e026049