SCOPING REVIEW
PERCEPTION OF PEDIATRIC ONCOLOGY PATIENTS ABOUT QUALITY OF LIFE IN PALLIATIVE CARE: SCOPING REVIEW
PERCEPÇÃO DE PACIENTES PEDIÁTRICOS ONCOLÓGICOS SOBRE QUALIDADE DE VIDA EM CUIDADOS PALIATIVOS: REVISÃO DE ESCOPO
PERCEPCIÓN DE PACIENTES PEDIÁTRICOS ONCOLÓGICOS SOBRE LA CALIDAD DE VIDA EN CUIDADOS PALIATIVOS: REVISIÓN DE ALCANCE
https://doi.org/10.31011/reaid-2026-v.100-n.2-art.2693
1Giovani Basso da Silva
2Heloísa Benvenutti
3Guilherme Kayser Prates
4Lucas Paulo de Souza
5 Maiara Rosa dos Santos
6João Gabriel Toledo Medeiros
7Luccas Melo de Souza
8 Lucia Campos Pellanda
1Mestrando no Programa de Pós-Graduação em Enfermagem da Universidade Federal de Ciências da Saúde de Porto Alegre, Porto Alegre, Brazil. ORCID: https://orcid.org/0009-0002-6915-4801
2Especialista em Atenção Cardiovascular. Fisioterapeuta. Hospital de Clínicas de Porto Alegre. Hospital de Clínicas de Porto Alegre, Porto Alegre, Brazil. ORCID: https://orcid.org/0000-0001-8558-1008
3 Graduando de enfermagem da Universidade Federal de Ciências da Saúde de Porto Alegre, Porto Alegre, Brazil. ORCID: https://orcid.org/0009-0002-6817-8991
4Mestrando no Programa de Pós-Graduação em Pediatria da Universidade Federal de Ciências da Saúde de Porto Alegre, Porto Alegre, Brazil. ORCID: https://orcid.org/0000-0002-3108-445X
5Mestre em Patologia pela Universidade Federal de Ciências da Saúde de Porto Alegre. Enfermeira, Porto Alegre, Brazil. ORCID: https://orcid.org/0000-0002-3108-445X
6Doutorando no Programa de Pós-Graduação em Pediatria da Universidade Federal de Ciências da Saúde de Porto Alegre, Porto Alegre, Brazil. ORCID: https://orcid.org/0000-0002-2789-9189
7Doutor em enfermagem e Professor do Departamento de Enfermagem da Universidade Federal do Rio Grande do Sul e do Programa de Pós-Graduação em Enfermagem da Universidade Federal de Ciências da Saúde de Porto Alegre, Porto Alegre, Brazil. ORCID: https://orcid.org/0000-0003-1629-9935
8Doutora em Ciências da Saúde. Médica e Professora da Universidade Federal de Ciências da Saúde de Porto Alegre, Porto Alegre, Brazil. ORCID: https://orcid.org/0000-0002-4593-3416
Corresponding Author
Guilherme Kayser Prates
Rua Sarmento Leite, 245- Porto Alegre, RS. Brazil. CEP: 90050-170. phone: +55 (51) 98152-9998. E-mail: guikprates@gmail.com
Submission: 20-11-2025
Approval: 07-04-2026
ABSTRACT
Objective: To explore how pediatric cancer patients who enter exclusive palliative care perceive their illness and quality of life, identifying the main factors influencing this experience. Method: This is a scoping review conducted according to the Joanna Briggs Institute guidelines and structured following the PRISMA-ScR checklist. Studies published between 2020 and 2025 were included, sourced from PubMed, Scielo, and Web of Science databases. Article selection was independently performed by two reviewers, with descriptive data analysis and methodological appraisal using a validated tool. Results: Of the 249 studies identified, 12 were included. The evidence revealed seven main categories: difference in perception between children and parents, symptoms and suffering, emotional and psychological aspects, impact of early palliative care introduction, advance care planning, perceived quality of life, and the importance of communication with professionals. Children often presented a more positive view than their parents, valuing autonomy and emotional support. Conclusion: Children’s perceptions of their condition should be taken into account in care decisions, reinforcing the importance of active listening, sensitive communication, and strategies that promote quality of life from the initiation of palliative care.
Keywords: Palliative Care; Child; Neoplasms; Oncology; Quality of Life.
RESUMO
Objetivo: Explorar como é a percepção de pacientes pediátricos com câncer que ingressam em cuidados paliativos exclusivos em relação à sua doença e qualidade de vida, identificando os principais fatores que influenciam essa vivência. Método: Trata-se de uma revisão de escopo conduzida conforme as diretrizes do JBI e estruturada segundo o checklist PRISMA-ScR. Foram incluídos estudos publicados entre 2020 e 2025, extraídos das bases PubMed, Scielo e Web of Science. A seleção dos artigos foi realizada de forma independente por dois revisores, com análise descritiva dos dados e avaliação metodológica por instrumento validado. Resultados: Do total de 249 estudos identificados, 12 foram incluídos. As evidências revelaram sete categorias principais: diferença na percepção entre crianças e pais, sintomas e sofrimento, aspectos emocionais e psicológicos, impacto da introdução precoce dos cuidados paliativos, planejamento antecipado de cuidados, qualidade de vida percebida e importância da comunicação com profissionais. Crianças frequentemente apresentaram uma visão mais positiva que seus pais, valorizando autonomia e suporte emocional. Conclusão: A percepção das crianças sobre sua condição deve ser considerada nas decisões de cuidado, reforçando a importância de uma escuta ativa, comunicação sensível e estratégias que promovam qualidade de vida desde a introdução dos cuidados paliativos.
Palavras-Chave: Cuidados Paliativos; Criança; Neoplasias; Oncologia; Qualidade de Vida.
RESUMEN
Objetivo: Explorar cómo es la percepción de los pacientes pediátricos con cáncer que ingresan a cuidados paliativos exclusivos en relación con su enfermedad y calidad de vida, identificando los principales factores que influyen en esta vivencia. Método: Revisión de alcance conforme a las directrices del Instituto Joanna Briggs y al checklist PRISMA-ScR. Se incluyeron estudios publicados entre 2020 y 2025, localizados en PubMed, Scielo y Web of Science. La selección fue realizada por dos revisores de forma independiente, con análisis descriptivo de los datos y evaluación metodológica mediante instrumento validado. Resultados: De los 249 estudios identificados, 12 fueron incluidos. Las evidencias se agruparon en siete categorías: diferencias de percepción entre niños y padres, síntomas y sufrimiento, aspectos emocionales, impacto de la introducción temprana de cuidados paliativos, planificación anticipada, calidad de vida percibida y comunicación con profesionales. Se observó que los niños tienden a expresar una visión más positiva que la de sus padres, con énfasis en la autonomía y el apoyo emocional. Conclusión: La percepción de los niños debe integrarse en las decisiones de cuidado, destacando la necesidad de comunicación sensible, escucha activa y estrategias que promuevan calidad de vida desde el inicio de los cuidados paliativos.
Palabras-Clave: Cuidados Paliativos; Niño; Neoplasias; Oncología; Calidad de Vida.
INTRODUCTION
Cancer represents one of the leading causes of morbidity and mortality among children and adolescents worldwide. Despite significant advances in oncological treatments, which have resulted in survival rates above 80% in developed countries, the therapeutic journey remains challenging for pediatric patients and their families(1).
However, a portion of these patients progress to advanced stages of the disease, requiring exclusive palliative care. At this stage, understanding children’s perception of their condition and quality of life becomes essential for the development of care strategies that address their specific needs(2).
Parents of children with cancer often perceive their children as vulnerable, which is associated with a poorer reported quality of life for the children. One study identified that parental perception of vulnerability negatively influences different aspects of children’s quality of life, including pain, nausea, procedural anxiety, worry, cognitive difficulties, and communication(3). These findings highlight the importance of considering parents’ perspectives when assessing children’s well-being, while also seeking strategies to minimize the impact of these perceptions on the child’s experience with the disease.
Emotional and psychological aspects, such as fear of death, resilience, and hope, also have a significant impact on these children’s experience. Strengthening continuous communication between caregivers and patients can serve as ongoing emotional support and also reduce levels of anxiety and depression(4). Such measures may promote the continuity of daily activities and the strengthening of family bonds, both during hospitalization for treatment and cure, and when “placing the patient under palliative care.”
The introduction of palliative care is hindered by sociocultural barriers that delay the family’s and the child’s understanding of their health-disease process(5). Integrating palliative care from the time of diagnosis allows for a more holistic approach, focused not only on treating the disease but also on the overall well-being of the child and family(5).
Given this context, this study aims to explore the perceptions of pediatric cancer patients receiving exclusive palliative care regarding their illness and quality of life, identifying the main factors that influence this experience. It also seeks to identify the main divergences and convergences, providing support for clinical practices that promote patient-centered care aligned with the needs of families and healthcare professionals.
METHODS
This is a literature review of the Scoping Review (SR) type. SRs are used to map the main concepts that support and guide a given field of research, as well as to clarify the working definitions and conceptual boundaries of a given topic(6).
This SR is structured in accordance with the Preferred Reporting Items for Systematic Review and Meta-Analysis Protocols (PRISMA-P) (7). PRISMA-P is a checklist designed to guide the development of a systematic review protocol, and its general concepts can be adopted in the preparation of an SR in order to ensure greater methodological rigor.
Protocol and registration
The SR was conducted in accordance with JBI guidance.8 The results were structured according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) checklist(7). The protocol for this SR was registered on the Open Science Framework platform under registration https://osf.io/h8u5e/.
Definition and alignment of the objective and research question
This SR aims to explore the perceptions of pediatric oncology patients who enter palliative care regarding their illness and quality of life. The formulation of the research question was guided by the PCC mnemonic (Population, Concept, and Context). Thus, the construction of the acronym considered: (1) as the population, children and adolescents diagnosed with cancer who entered exclusive palliative care; (2) as the concept, the perception of illness and quality of life reported by the patients themselves, parents, or caregivers, as well as their experiences in palliative care; and (3) as the context, studies addressing the experiences of pediatric patients in palliative care, considering different care settings, such as hospitals, homes, and specialized units.
Based on the definition of the mnemonic, the following research question was developed: “What are the perceptions of pediatric oncology patients who enter exclusive palliative care regarding their illness and quality of life?”
Inclusion and exclusion criteria
The inclusion criteria for this review comprised primary studies (such as randomized clinical trials, cohort studies, cross-sectional studies, observational studies, among others) and secondary studies (systematic reviews, integrative reviews, meta-analyses, among others). Only published studies in English, indexed in journals, from January 2020 to February 2025, the month in which the studies were collected, were considered eligible. This study excluded studies conducted outside the hospital context, as well as research involving neonatal, adult, or geriatric populations.
Search strategy
Based on the PCC mnemonic, the search strategies were developed using DeCS/MeSH Terms in Portuguese, English, and Spanish. The search strategy is systematized in Chart 1. The search was conducted in the PubMed, SciELO, and Web of Science databases between January and February 2025.
Chart 1 - Search strategies. Porto Alegre, Rio Grande do Sul, 2025.
|
Database |
Search strategy |
Results (n) |
|
PubMed |
((Child OR Children OR Pediatric OR Pediatrics OR Childhood) AND (Cancer OR Neoplasms OR Oncology OR Pediatric Oncology OR Childhood Cancer) AND (Palliative Care OR Pediatric Palliative Care OR End-of-Life Care OR Terminal Care) AND (Quality of Life OR Well-Being OR Health Perception OR Psychosocial Aspects) AND (Perception OR Patient Perception OR Perspective OR Patient Experience OR Attitudes)) |
3 |
|
SciELO |
((Child OR Children OR Pediatric OR Pediatrics OR Childhood) AND (Cancer OR Neoplasms OR Oncology OR Pediatric Oncology OR Childhood Cancer) AND (Palliative Care OR Pediatric Palliative Care OR End-of-Life Care OR Terminal Care) AND (Quality of Life OR Well-Being OR Health Perception OR Psychosocial Aspects) AND (Perception OR Patient Perception OR Perspective OR Patient Experience OR Attitudes)) |
4 |
|
Web of Science |
TS=((Child OR Children OR Pediatric OR Pediatrics OR Childhood) AND (Cancer OR Neoplasms OR Oncology OR Pediatric Oncology OR Childhood Cancer) AND (Palliative Care OR Pediatric Palliative Care OR End-of-Life Care OR Terminal Care) AND (Quality of Life OR Well-Being OR Health Perception OR Psychosocial Aspects) AND (Perception OR Patient Perception OR Perspective OR Patient Experience OR Attitudes)) |
242 |
Source: Authors (2025).
Study selection
After the search in the databases, all stages of the selection of eligible studies were carried out systematically, in pairs, independently, and blinded by two different researchers, as recommended by the JBI, using the Rayyan® tool(8). Any disagreements identified were resolved by a third reviewer. The study inclusion process was systematized and conducted in accordance with the PRISMA Checklist, and it is presented in the results section(7).
Data extraction
Data extraction was carried out systematically and in a standardized manner, using Microsoft Excel® software to ensure the consistency and reproducibility of the SR. The following study information was summarized: title, author, year, country of origin, objective, design, and main findings.
Data analysis
The analysis of the evidence was carried out through the organization and structured presentation of the extracted data. To this end, tables, graphs, and visual representations were used in order to optimize the intelligibility of the findings presented descriptively. The selected studies were also analyzed for quality using the JBI Checklist for Analytical Cross Sectional Studies(8). Aspects such as the definition of subjects and settings, the validity and reliability of exposure measurement, the adequacy of diagnostic criteria, the identification and control of confounding factors, the validity and reliability of outcome measurements, and the appropriate use of statistical analysis were evaluated. Studies that met more than 90% of these criteria were classified as high quality(9). For the assessment of risk of bias and methodological quality of the studies, the Robvis Online tool was used, adapted according to JBI recommendations(8,10).
RESULTS
A total of 249 studies were identified through searches of the PubMed (n=3), SciELO (n=4), and Web of Science (n=242) databases, using the previously defined strategies. After duplicate removal with the aid of the Rayyan software, 247 records remained for title and abstract screening. At this stage, 220 studies were excluded for not meeting the eligibility criteria. Then, 27 articles were selected for full-text reading. After this complete assessment, 15 records were excluded for not meeting the inclusion criteria. Thus, 12 studies comprised the final sample of this study, as presented in Figure 1.
Figure 1 - Flowchart of the selection of eligible studies. Porto Alegre, Rio Grande do Sul, 2025.
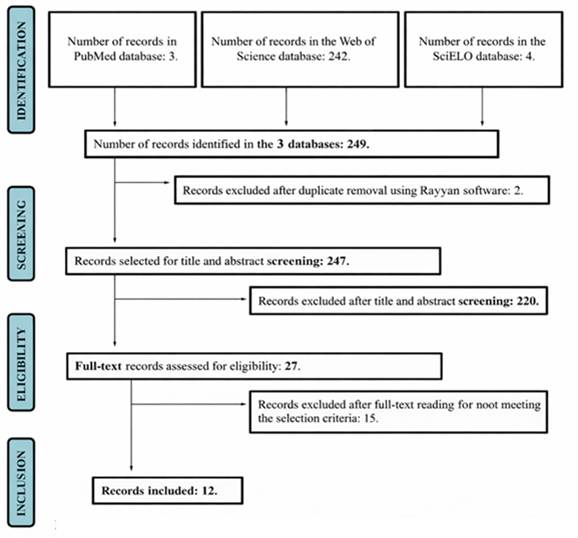
Source: Authors, 2025.
Characteristics of the studies
The studies included in this review were published between 2019 and 2024, with the highest concentration in 2024 (n=4). The United States was the country with the highest number of publications (n=5), followed by Spain (n=2), while the remaining countries (India, China, Italy, South Korea, and Canada) contributed one study each. Most studies were conducted in North American countries, totaling seven studies, which reflects a trend of scientific production concentrated in this region. The study samples ranged from 10 to 159 participants, with the largest sample observed in the study conducted in Canada. Chart 2 describes the main characteristics of the studies.
In addition, the methodological quality of the studies was assessed based on the JBI Checklist for Analytical Cross Sectional Studies instrument(8). Chart 2 presents a synthesis of the methodological quality assessment of the included studies, indicating the criteria met by each one. Additionally, Figure 2 shows the Quality Assessment and Risk of Bias of the studies, allowing a comparative visualization of the results obtained from the application of the checklist.
Chart 2 - Articles selected to compose the review. Porto Alegre, Rio Grande do Sul, 2025.
|
Study |
Year |
Location |
Sample |
Criteria Met (%) |
Classification |
|
Montgomery (2020) (11) |
2020 |
USA |
46 |
95 |
High Quality |
|
Toro-Pérez (2024) (12) |
2024 |
Spain |
44 |
90 |
High Quality |
|
Requena (2022) (13) |
2022 |
USA |
23 |
85 |
Moderate Quality |
|
Suthan (2024) (14) |
2024 |
India |
75 |
88 |
High Quality |
|
Montgomery (2019) (15) |
2019 |
USA |
46 |
93 |
High Quality |
|
Lin (2023) (16) |
2023 |
China |
10 |
80 |
Moderate Quality |
|
Podda (2021) (17) |
2021 |
Italy |
41 |
87 |
Moderate Quality |
|
Kim (2021) (18) |
2021 |
South Korea |
109 |
92 |
High Quality |
|
Kaye (2021) (19) |
2021 |
USA |
32 |
89 |
High Quality |
|
Toro-Pérez (2024) (20) |
2024 |
Spain |
30 |
91 |
High Quality |
|
Bedoya (2022) (21) |
2022 |
USA |
129 |
84 |
Moderate Quality |
|
Johnson (2024) (22) |
2024 |
Canada |
159 |
88 |
High Quality |
Source: Research data, 2025.
Figure 2 - Quality Assessment and Risk of Bias of the Studies.
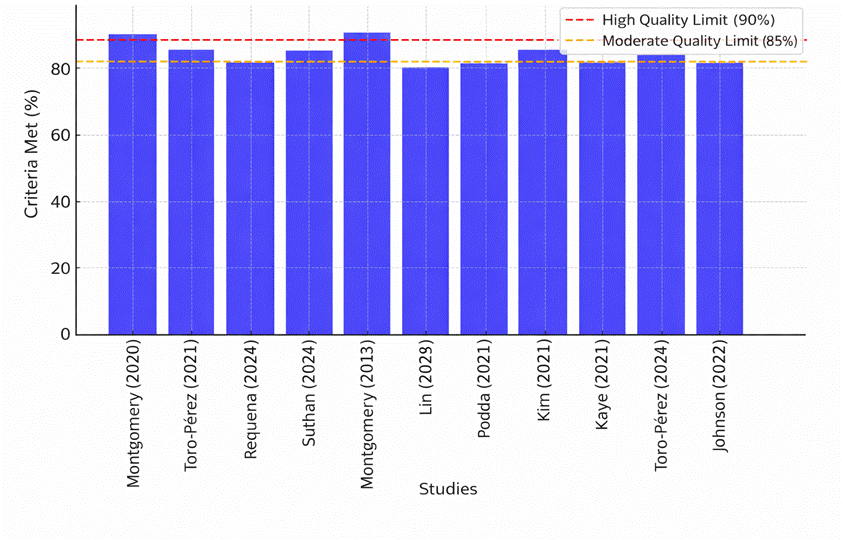
Source: Research data, 2025.
In order to establish the main risk factors and possible biases, the authors analyzed the included studies based on the criteria of the adopted checklist. Four main categories of methodological risk were identified. The first factor refers to sample representativeness, since some studies presented small sample sizes or restricted selection, which may compromise the generalizability of the results(16,21). The second factor concerns the measurement of exposure, especially in studies that did not clearly describe the data collection procedures related to patients’ perception of quality of life(13).
The third critical point was the identification of confounding factors; in several studies, robust strategies were not adopted to control information and selection biases, which may compromise the validity of the conclusions(13,14,16,17,19,21). A deficiency in statistical analysis was observed in studies with lower methodological scores, which presented less sophisticated statistical analyses or did not perform adjustments for potential biases(16,21).
Finally, the studies were organized into thematic groups based on the similarities identified in the perceptions expressed by the children regarding their own illness, considering emotional, cognitive, social, and existential aspects emerging from their reports. Chart 3 systematically presents the main themes identified in the included studies, illustrating the principal findings.
Chart 3. Main findings identified. Porto Alegre, Rio Grande do Sul, 2025.
|
Theme |
Main Findings |
Referenced Studies |
|
Difference in Perception between Children and Parents |
Children assess their quality of life more optimistically than their parents. |
Montgomery (2020) (11) Toro-Pérez (2024) (12) |
|
Symptoms and Suffering |
The most frequently reported symptoms include pain, fatigue, and difficulty sleeping. |
Requena (2022) (13) Montgomery (2019) (15) |
|
Emotional and Psychological Aspects |
Children express fear of separation, but also demonstrate resilience. |
Lin (2023) (16) Kim (2021) (18) |
|
Impact of Early Introduction of Palliative Care |
It improves the adaptation of patients and their families. |
Podda (2021) (17) Kaye (2021) (19) |
|
Discussions on Advance Care Planning |
Adolescents reported that discussions on advance care planning improved their communication with family members and friends. |
Bedoya (2022) (21) |
|
Quality of Life Perceived by Children with Advanced Cancer |
Children highlight the importance of maintaining autonomy, establishing normality, and receiving emotional support. |
Johnson (2024) (22) |
|
Importance of Communication and Relationship with Healthcare Professionals |
Children value open communication and emotional support. |
Suthan (2024) (14) Toro-Pérez (2024) (20) |
Source: Research data, 2025.
DISCUSSION
The perception of pediatric oncology patients who enter exclusive palliative care regarding their illness and quality of life is a sensitive topic that remains underexplored in healthcare settings. Attention is often focused on the perspectives of healthcare professionals and family members, while the child’s own perspective is neglected. However, in the context of pediatric oncology, it is essential that the child has a voice and is understood in relation to their health-disease process(23).
When assessing the perception of children with cancer regarding exclusive palliative care, this study identified seven themes of greatest relevance to this population, highlighting the need to consider their experiences and feelings in the care approach.
Difference in Perception between Children and Parents
Some studies identified that children with advanced cancer often assess their quality of life more optimistically than their parents or caregivers, even in the presence of severe symptoms(11-12). This observation is supported by a study conducted in Portugal, which found a more positive perception among children compared to their parents, indicating moderate agreement between self-report and proxy report(24). These discrepancies may be attributed to the parents’ intense emotional involvement and their desire to protect their children, which may distort the perception of the children’s actual suffering. Understanding these differences is crucial to align therapeutic approaches and ensure that the children’s real needs are met(25).
Children facing oncological diseases often demonstrate early maturity due to post-traumatic stress situations, adopting more mature behaviors and losing part of the typical experience of childhood(25-26). This characteristic may be related to the desire to protect their family members, leading them to minimize or conceal their true feelings about their health and illness.
Symptoms and Suffering
In contrast, when themes related to symptomatology and suffering in relation to their health-disease process were addressed, it was identified that the symptoms most frequently reported by children with advanced cancer include pain, fatigue, difficulty sleeping, and loss of appetite(13,15). These findings are consistent with a study showing that hospitalized children and adolescents with cancer present low quality of life and high levels of fatigue(17,27).
However, in some cases, even under palliative care, many children continue to experience symptoms that are not fully controlled. The persistent presence of these symptoms may result from inadequate management approaches or from the natural progression of the disease (28). Therefore, it is essential that healthcare teams regularly assess symptoms and adjust therapeutic interventions as needed in order to provide effective relief(23).
Emotional and Psychological Aspects
The emotional aspects of children with cancer receiving palliative care are also an extremely important theme and should be continuously assessed throughout the exclusive palliative care process. Some studies identified that children with advanced cancer express fear of separation from family members, but also demonstrate resilience and hope(16,18). These children often wish to continue normal activities, such as playing and interacting socially. A study on the perceptions of pediatric and adolescent oncology patients highlighted the importance of continuous emotional support, showing that children who receive this support present lower levels of anxiety and depression(29).
Children may develop a feeling that makes them feel responsible for their family members. A study addressing the experiences of siblings of children with cancer emphasized that adequate emotional support is essential for the psychological well-being not only of the patient, but of the entire family(30). In view of this, it is essential to consider that interventions promoting the continuity of daily activities and the strengthening of family bonds may contribute to the resilience and quality of life of these children.
Impact of the Early Introduction of Palliative Care
Perceptions of palliative care vary among those involved, including healthcare professionals, patients, and family members. What may seem like an early approach to some may represent an essential need at the right moment for others. The early introduction of palliative care improves adaptation to the diagnosis and treatment of pediatric patients and their families(17,19). This early approach is associated with a greater likelihood of patients dying at home rather than in hospitals. A study on pediatric palliative care reinforces that early health education regarding palliative care facilitates greater participation of the child in decisions about their own treatment(31).
Integrating palliative care from the time of diagnosis allows for a more holistic approach, focused not only on treating the disease but also on the overall well-being of the child and the family. There are several ways to address this topic, whether through conversations directed at the patient or through the use of therapeutic play, promoting a better quality of life and a more shared decision-making process(25).
Discussions on Advance Care Planning
Within pediatric groups, adolescents reported that discussions about advance care planning improved communication with family members and friends. However, many parents and healthcare professionals remain reluctant to address the topic, despite children’s desire to be included in decisions about their health(21). A review on pediatric palliative care highlights the importance of including children and adolescents in discussions about their care plan, respecting their autonomy and potentially reducing anxiety related to the unknown, while improving their acceptance of the disease(32).
Perceived Quality of Life in Children with Advanced Cancer
Children with advanced cancer highlight the importance of maintaining autonomy, establishing a sense of normality, and receiving emotional support(22). These findings are supported by other studies that describe the health-related quality of life of children with cancer, emphasizing that social support and a sense of belonging are factors that positively impact the perception of quality of life(27,29-30). Strategies that encourage children’s active participation in everyday and therapeutic decisions, as well as the maintenance of family and school routines, may significantly improve their quality of life.
Importance of Communication and Relationships with Healthcare Professionals
It is essential that the child’s voice be considered in the care process, fostering the development of bonds among healthcare professionals, patients, and family members, with emphasis on open communication and the emotional support offered by the care team(14,20). The presence of multidisciplinary teams contributes to more humanized and comprehensive care(25,33). Effective communication among the healthcare team, the child, and the family is essential to build trust and ensure that the child’s needs and wishes are fully understood and addressed.
FINAL CONSIDERATIONS
This study reviewed the scientific literature to understand how children with advanced cancer perceive their illness and quality of life when entering exclusive palliative care. The analysis of the 12 included studies revealed that children’s perception of their condition varies widely and is influenced by factors such as pain and other symptom control, emotional support, communication with healthcare professionals, and the maintenance of autonomy.
It is noteworthy that, although parents often overestimate their children’s suffering, the children themselves, in many cases, present a more optimistic view of their quality of life. This finding reinforces the need to actively include children in discussions about their care, respecting their cognitive ability to understand and express their preferences.
The literature also shows that the early introduction of palliative care improves the adaptation of children and their families, reducing unnecessary suffering and ensuring greater dignity throughout the course of the disease. However, challenges remain in the implementation of this care, especially due to the reluctance of professionals and family members to discuss disease progression and advance care planning.
Thus, this study reinforces the importance of open and sensitive communication between healthcare teams and pediatric patients, as well as the need for individualized strategies for symptom control and emotional support. Expanding access to pediatric palliative care and training multidisciplinary teams are essential measures to ensure that these children live with quality and dignity.
Finally, it is suggested that future research further explore the perspective of the patients themselves regarding the psychological and social aspects of the palliative experience, seeking methodologies that give children an active voice, in order to guide increasingly humanized and patient-centered care policies.
REFERENCES
1 Guedes AKC, Pedrosa APA, Osório MO, PedrosaTF. Cuidados paliativos em oncologia pediátrica: perspectivas de profissionais de saúde. Rev SBPH [Internet]. 2019 [citado 2023 out 28];22(2):128-48. Disponível em: http://pepsic.bvsalud.org/scielo.php?script=sci_arttext&pid=S1516- 08582019000300008&lng=pt
2 Momani TG, Mandrell BN, Gattuso JS, West NK, Taylor SL, Hinds PS. Children's perspective on health-related quality of life during active treatment for acute lymphoblastic leukemia: an advanced content analysis approach. Cancer Nurs. 2015 Jan-Feb;38(1):49-58. doi: https://doi.org/10.1097/NCC.0000000000000174
3 Azak M, Ekinci B, Barış S, Yildiz S. The influence of parental perceptions of vulnerability on quality of life in pediatric cancer patients aged 5-7 years. J Pediatr Nurs. 2025 Feb 7:S0882-5963(25)00042-9. doi: https://doi.org/10.1016/j.pedn.2025.01.031
4 Kenney AE, Bedoya SZ, Gerhardt CA, Young-Saleme T, Wiener L. End of life communication among caregivers of children with cancer: A qualitative approach to understanding support desired by families. Palliat Support Care. 2021 Dec;19(6):715-722.doi: https://doi.org/10.1017/S1478951521000067
5 Ehrlich BS, Movsisyan N, Batmunkh T, Kumirova E, Borisevich MV, Kirgizov K, et al. Barriers to the early integration of palliative care in pediatric oncology in 11 Eurasian countries. Cancer. 2020 Nov 15;126(22):4984-4993. doi: https://doi.org/10.1002/cncr.33151
6 Peters MDJ, Godfrey C, McInerney P, Munn Z, Tricco AC, Khalil, H. Chapter 11: Scoping Reviews (2020 version). In: Aromataris E, Munn Z. JBI Manual for Evidence Synthesis, JBI, 2020. doi: https://doi.org/10.46658/JBIMES-20-12
7 Shamseer L, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015: elaboration and explanation. BMJ 2015; 349:g7647 doi: https://doi.org/10.1136/bmj.g7647
8 Joanna Briggs Institute: Checklist for Analytical Cross-Sectional Studies [Internet]. 2017 [cited in 2023 set 22]. Avaliable from: https://jbi.global/sites/default/files/2019-05/JBI_Critical_Appraisal-Checklist_for_Analytical_Cross_Sectional_Studies2017_0.pdf
9 Barker TH, et al. Revising the JBI quantitative critical appraisal tools to improve their applicability: an overview of methods and the development process. JBI Evidence Synthesis. 2023;21(3). doi: https://doi.org/10.11124/jbies-22-00125
10 McGuinness, LA, Higgins, JPT. Risk-of-bias VISualization (robvis): An R package and Shiny web app for visualizing risk-of-bias assessments. Res Syn Meth. 2021; 12: 55–61. doi: https://doi.org/10.1002/jrsm.1411
11 Montgomery KE, et al. Comparison of child self-report and parent proxy-report of symptoms: results from a longitudinal symptom assessment study of children with advanced cancer. J Spec Pediatr Nurs. 2020;25(3):e12316. doi: https://doi.org/10.1111/jspn.12316
12 Toro-Pérez D, et al. Evaluating quality of life in pediatric palliative care: a cross-sectional analysis of children’s and parents’ perspectives. Eur J Pediatr. 2024;183:1305-14. doi: https://doi.org/10.1007/s00431-023-05330-4
13 Requena ML, Avery M, Feraco AM, Uzal LG, Wolfe J, Dussel V. Normalization of symptoms in advanced child cancer: the PediQUEST-Response case study. J Pain Symptom Manage. 2022;63(4):548-62. doi: https://doi.org/10.1016/j.jpainsymman.2021.12.009
14 Pandarakutty S, Arulappan J. Health-related quality of life of children and adolescents with sickle cell disease: an evolutionary concept analysis. Appl Nurs Res. 2024;80:151862. doi: https://doi.org/10.1016/j.apnr.2024.151862
15 Montgomery KE, et al. Using patient-reported outcomes to measure symptoms in children with advanced cancer. Cancer Nurs. 2019;43(4):281-9. doi: https://doi.org/10.1097/NCC.0000000000000721
16 Lin N, Lv D, Hu Y, Zhu J, Xu H, Lai D. Existential experiences and perceptions of death among children with terminal cancer: an interpretative qualitative study. Palliat Med. 2023;37(6):866-74. doi: https://doi.org/10.1177/02692163231165100.
17 Podda M, et al. Customised pediatric palliative care: Integrating oncological and palliative care priorities. Acta Paediatr. 2021; 110: 682–688. doi: https://doi.org/10.1111/apa.15415
18 Kim JY, Park BK. The most important aspects for a good death: perspectives from parents of children with cancer. Inquiry. 2021;58:469580211028580. doi: https://doi.org/10.1177/00469580211028580
19 Kaye EC, et al. The impact of specialty palliative care in pediatric oncology: a systematic review. J Pain Symptom Manage. 2021;61(5):1060-79.e2. doi: https://doi.org/10.1016/j.jpainsymman.2020.12.003
20 Toro-Pérez D, Camprodon-Rosanas E, Navarro Vilarrubí S, Bolancé C, Guillen M, Limonero JT. Assessing well-being in pediatric palliative care: A pilot study about views of children, parents and health professionals. Palliat Support Care. 2024;22(5):1000-8. doi: https://doi.org/10.1017/S1478951523000251.
21 Bedoya SZ, et al. Adolescent and young adult initiated discussions of advance care planning: family member, friend and health care provider perspectives. Front Psychol. 2022;13:871042. doi: https://doi.org/10.3389/fpsyg.2022.871042
22 Johnson A, Ali R, An E, Wilson C, Widger K. Children’s and adolescents’ perspectives on living with advanced cancer: a meta-synthesis of qualitative research. Qual Life Res. 2024;33:2095-106. doi: https://doi.org/10.1007/s11136-024-03688-y
23 Souza LP, Santos DP, Carvalho GP, Barbosa JS, Vinholes DB, Viana ACW. Análise da qualidade de vida em crianças e adolescentes sob tratamento oncológico. Rev. Soc. Bras. Enferm. Ped. 2023;23:eSOBEP20230032. doi: http://dx.doi.org/10.31508/1676-379320230032
24 Batalha LMC, Fernandes AM, Campos C de. Qualidade de vida em crianças com câncer: concordância entre crianças e pais. Esc Anna Nery [Internet]. 2015Apr;19(2):292–6. doi: https://doi.org/10.5935/1414-8145.20150039
25 Silva GB da, Souza LM de, Canabarro ST. Construção e validação de História em Quadrinhos para crianças com leucemia linfoide aguda. Esc Anna Nery [Internet]. 2024;28:e20220419. doi: https://doi.org/10.1590/2177-9465-EAN-2022-0419pt
26 Murphy KM, Siembida E, Lau N, Berkman A, Roth M, Salsman JM. A systematic review of health-related quality of life outcomes in psychosocial intervention trials for adolescent and young adult cancer survivors. Crit Rev Oncol Hematol. 2023 Aug;188:104045. doi: https://doi.org/10.1016/j.critrevonc.2023.104045
27 Nunes MDR, Jacob E, Lopes-Júnior LC, Leite ACAB, Lima RAG de, Nascimento LC. Qualidade de vida da população infantojuvenil oncológica com e sem fadiga. Acta paul enferm [Internet]. 2022;35:eAPE0288345. doi: https://doi.org/10.37689/acta-ape/2022AO0288345
28 Diaz Osorio CE, Carmona Mejía B, Bárcenas Bobadilla L, Ponce Gómez G. Necesidades de cuidados paliativos en niños con diagnóstico oncológico en un hospital de tercer nivel de atención: Palliative care needs in children with oncological diagnosis in a tertiary care hospital. LATAM [Internet]. 2024 Aug 9 [cited 2025 Feb 24];5(4):3174–83. Available from: https://latam.redilat.org/index.php/lt/article/view/2489
29 Thornton CP, Ruble K, Kozachik S. Psychosocial interventions for adolescents and young adults with cancer: an integrative review. J Pediatr Oncol Nurs. 2020 Nov-Dec;37(6):408-22. doi: https://doi.org/10.1177/1043454220919713
30 Giesta DM, Azambuja TO, Moreira MC. Convivendo com uma nova realidade: revisão sistemática da literatura sobre as experiências dos irmãos de crianças com câncer. Psicol Hosp (São Paulo) [Internet]. 2018 [cited 2025 Feb 24];16(1):67-89. Available from: https://www.academia.edu/113924442/Convivendo_com_uma_nova_realidade_revis%C3%A3o_sistem%C3%A1tica_da_literatura_sobre_as_experi%C3%AAncias_dos_irm%C3%A3os_de_crian%C3%A7as_com_c%C3%A2ncer?uc-sb-sw=109505750
31 Lima SF, Lamy ZC, Motta VBR da, Roma TM, Gomes CMR de P, Souza T de P. Dinâmica da oferta de cuidados paliativos pediátricos: estudo de casos múltiplos. Cad Saúde Pública [Internet]. 2020;36(9):e00164319. doi: https://doi.org/10.1590/0102-311X00164319
32 Costa TF da, Ceolim MF. A enfermagem nos cuidados paliativos à criança e adolescente com câncer: revisão integrativa da literatura. Rev Gaúcha Enferm [Internet]. 2010Dec;31(4):776–84. doi: https://doi.org/10.1590/S1983-14472010000400023
33 Paiani RL, Pereira TB, Poggetti IR, Wissmann LH, Alves AA, Bittencourt ACO, et al. Aspectos psicológicos de pais de crianças e adolescentes em cuidados paliativos: uma revisão integrativa. Rev SBPH [Internet]. 2022 Dec [cited 2025 Mar 5];25(2):55-67. Available from: https://revistasbph.emnuvens.com.br/revista/article/view/485
Funding and Acknowledgments:
This research received no funding.
Authorship Criteria (Author Contributions)
All the authors listed above contributed significantly to: 1. the conception and/or planning of the study; 2. the acquisition, analysis, and/or interpretation of the data; 3. as well as the drafting and/or critical review and final approval of the published version.
Data Availability Statement
No databases were generated in this study. The information presented is described in the body of the article. Conflict of Interest Statement Nothing to declare.
Scientific Editor: Ítalo Arão Pereira Ribeiro. Orcid: https://orcid.org/0000-0003-0778-1447
Rev Enferm Atual In Derme 2026;100(2): e026044